
Yesterday afternoon another young doctor jumped to her death in NYC. She landed at the entrance of the building where she lived.
Within less than an hour, I received the following emails about her. All published with permission.
“Hello Pamela, I am not a doctor, but a mother of 3 and a wife of an resident physician. Tonight I watched AGAIN the police taking the body of another female doctor—lifeless—into a body bag. Two doctors died from jumping off our 33-story building in 2 years and no one seems to care. The hospital and everyone is so silent. They cover it up. No one talks about. Someone dies and everyone puts their heads down and ignores it and are told by the hospital to keep quiet—especially to reporters.
Thank you so much for your blog, public speaking, and advocacy. Since I’m not a doctor, there’s only so much I can understand about what my husband is going through. Discovering your blog has helped me know how to help my husband in so many ways. I worry so much about him. When we’ve tried to seek mental health care, we’ve had to be top secret about it. It’s insane. I’m tired of seeing dead bodies out my window. I’m tired of being on the sidelines. I’m feeling so angry and upset. I feel so powerless. What actions can I take to make sure I never see something like this happen again? Words can never describe how it feels to see a dead body outside your window. A beautiful lifeless body of a beautiful doctor.
This is what I saw when I came home tonight—a dead doctor lying under that tarp—lifeless in the freezing cold. What I am suppose to tell my daughter when she asks, ‘Mommy what’s that?’”

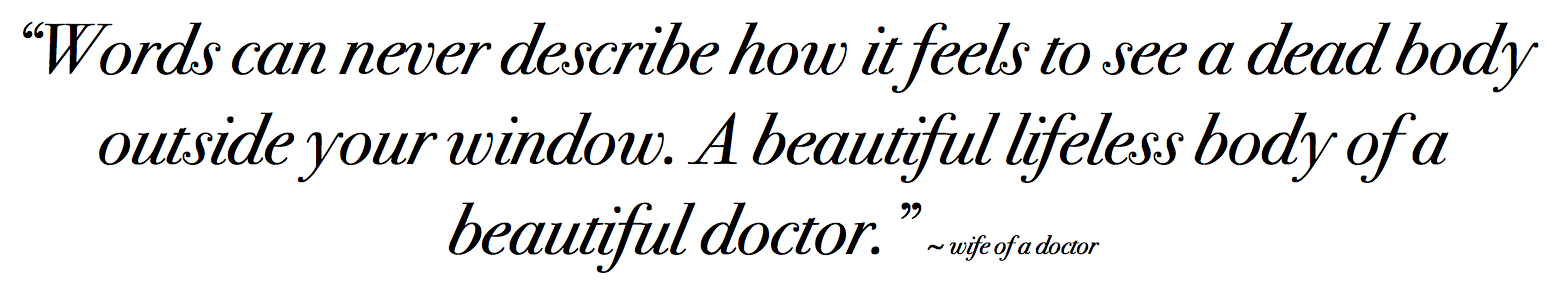 Email #2
Email #2
“I’m a physician. I have a career ahead of me, which I’m too scared to speak out against. I came home again to another suicide. Another doctor dead from Mt. Sinai in NY. I think NY is a horrible place to work. Conditions are deplorable for doctors and you should investigate. Both suicides were horrible—jumped from our high rise. I’m convinced it’s the exhaustion, the demands to perform at 100% 24/7 to meet ridiculous administrative and FINANCIAL demands. We need to change healthcare. In NY doctors are blamed for everything the nurses, techs, janitors, staff don’t do. We have to do every job AND document and be nice 100% of the time. Everyone is protected by unions—except doctors. We’re criticized and destroyed with unbelievable debt. I don’t know why anyone would willingly go into this field. I love what I do, but I have grown to hate this system. I have lived in a culture of shame for too long. Would you please expose these Manhattan hospitals? They lack compassion. They are all obsessed with finances, prestige and scores. This suicide today was horrific. I came into my building—a crime scene. Don’t let another doctor’s life go unspoken for. They will likely say she was troubled, but why was she troubled!?? Because she wasn’t efficient enough? Sad and overworked? Our hospital will make it about her. Like the girl that died last year, she was too sad.”
Then I got an email that truly shocked me.
I do not have permission to publish this one so I won’t. I will say that it came from a man who I deeply admire, a man who is a health system executive in NYC. He wrote me in distress about the loss of this young doctor. He explained that hospitals investigate why things go wrong in patient care and lessons learned are shared to improve processes and prevent future deaths. When a doctor dies by suicide, how are we to learn from this tragedy if we don’t study what went wrong? Police don’t investigate suicides. Investigation is left to grieving family and friends. Don’t we have an obligation as a society and as medical professionals to understand why these suicides occur? He concludes, “If this were a patient, we’d be all over it and so would the regulators.”
A few hours before this flurry of emails, I was on the phone with a doctor who reported that her own family physician shot herself in her clinic. The doctor who called me disclosed the she had never been suicidal herself—except once, during residency for about 15 minutes. In an impulsive move she went up to the roof of her 5-story hospital. Standing on the ledge, she recalled a lecture in which she was instructed that to assure death one must jump from at least 6 stories. So she paused. Then turned around and went back to work.
Now to answer the questions posed to me by the doctor’s wife, the physician, and the hospital executive. First, I believe we all have a common goal—to end these suicides.
To the wife of the resident physician who asks, “What actions can I take to make sure I never see something like this happen again?” I say talk about these suicides. Secrets will not save us. Organize a support group for physicians and their spouses. Don’t wait for another fallen physician. Channel your passion into action. Reach out to others in your building in a way that inspires and fuels you.
To the doctor who asks, “Would you please expose these Manhattan hospitals?” I say that as doctors we must all speak up about injustice, human rights violations in medical education, and deplorable working conditions in our first-world hospitals. It’s not just Manhattan hospitals. Doctors and medical students are dying by suicide throughout the United States and the world. This is a global epidemic.
To the executive who asks, “Don’t we have an obligation as a society and as medical professionals to understand why these suicides occur?” I say yes. I hold our medical system to the highest standard when it comes to protecting human life—and that includes the lives of our doctors. As a society we must understand that this is a public health crisis. More than one million Americans lose their doctors to suicide each year. We can no longer cover up these deaths with tarps and silence. We can no longer walk away from the very people who have dedicated their lives to serving others. It’s just wrong.
“How are we to learn from this tragedy if we don’t investigate?” Without an investigation, history will repeat itself. More doctors will plunge to their deaths from hospitals and resident housing complexes in NYC. If we don’t investigate this death, we are each complicit in the loss of future physicians to suicide. Now is the time for fearless leadership, for the heroes among us to reveal themselves and take a stand for our doctors—for the men and women who walk into our hospitals everyday to so selflessly serve others.
My question to you is “What will you do to prevent the next doctor suicide?
Need help?
Physician Suicide 101: Secrets, Lies & Solutions
What I’ve learned from 757 doctor suicides
Addendum: Doctors were working in the hospital right next to this building and could see there was a woman preparing to jump. They witnessed her fall. They knew she could be one of their friends (since the building houses primarily doctors). Yet these doctors had to continue to care for patients amid their tears and screams at the window. Many have flashbacks to colleagues that jumped from same building in previous years. “It is always the same thing,” says one resident. The hospital sends the usual ‘we’ve had a tragic death’ email. They tell us to meditate, sleep, and hydrate.” Then it happens again.
~~~
Please also read My eulogy to Dr. Deelshad Joomun and Doctor suicide: where are the vigils, cards & flowers? Refinery29 reports This hospital has a physician suicide problem.















Thank you from the bottom of my heart, Dr. Pamela Wible, for your passion and purpose and never giving up, and encouraging others to speak out and change the sick and dysfunctional system that we have.
I still remember my residency in family medicine, over 40 years ago, as one of the worst times of my life. Now my son is an emergency physician and his wife in her fourth year of OB/GYN residency, and I actually moved to their city, just to be close and be a support to them and their little children. I am so proud of them, and they created a good circle of strong supportive friendships, and their university setting in the Midwest is, from my observation, less harsh than the ones I lived in and was familiar with on the East Coast.
Compassion needs to be Central in medical training (it is not!), and needs to start with compassion for the Physicians themselves. I have no doubt that more women being in leadership in academics will be of some help, but the basic patriarchal non-compassionate system can also suck them in, as I have seen.
I love that you are creating exposure of this huge, shameful problem, encouraging others to do the same. I will add my voice in anyway I can.
I wish there were a way that I could be part of a hotline and actually talk with young physicians in crisis, I would not want to be the only one doing this obviously, but I would be happy to be part of a pool of such people. My heart is right there with them, and with your work.
Sincerely, Candace Corson, M.D.
Thanks Candace! You can help just by reaching out to others where you live. Offer to be a residency “mom” ad help out the residents with things they need (as sort of a secret way in to bond with them). No need to do exactly what I’m doing. Just help the med students and doctors who are in the 5 mile radius of where you are reading this comment now.
These girls died, and no one is looking at what happened. If you’re dealing w depression or burnout- they say call this number- AND then get labeled. You’re unprofessional for being human, for feeling anything other than getting your job done FAST. I know for a fact the other girl reached out to the resident union before she died (we have a resident union, but it’s for bargaining salary and benefits, doesn’t actually protect your job, it is very easy (as others have pointed out) to say that anyone that is dealing with anything (family issues, depression, medical problems) is unprofessional, and there is no protection from that. I don’t know why she went to the union but no one goes to the union unless they’re having residency problems. Also- both girls were dept of medicine. I think nice people, but incredibly overworked with very little support staff (residents are often forced to take care of nursing tasks that are not done in a timely way, social work, along with their own duties).
Pamela, I am so disheartened to learn of this. It’s clear that a more emphatically direct approach needs to be taken at Mount Sinai hospital (and all others) to compel accountability and promote programs that provide genuine support.
Physicians and their spouses and concerned family members need to write to key leaders at Mt. Sinai and demand that they investigate physician suicide by appointing a task force of experts drawn from within and outside of the hospital who will study not only this suicide but the issue of physician suicides more broadly and explore best practices, and whose report will be made publicly available.
Mt. Sinai’s CEO, Chairman of the Board and all board members as well as the Chief Medical Officer, President of the Medical Staff, Director of Residency Programs and director of that specialty’s department each need to be written and asked specifically how they are going to respond to this. How are they going to investigate not only this physician’s suicide but the problem of burnout, depression and suicides amongst physicians within their institutions.
Someone needs to identify by name each of these key players and their addresses and publicly share this in whatever forum is possible, for example this blog comment section. Then each concerned person needs to write to each and everyone of them demanding a response. They need to be held accountable by name. It will help if the writer lets it be known that they know that others are writing as well and that amongst those observing the developments are journalists who are closely following the story. It wouldn’t hurt to let that recipient know the names of the others you’ve written to and encouraging them to connect.
Additionally, a supportive note of condolence ought to be sent to the spouse or parent of the physician. Individual grief counseling needs to be provided. A process similar to critical incident stress management ought to be made available to help people process as a group what happened. In addition to decompressing the stress build-up which ultimately contributes to suicide contagion, it enables people to come together as a community, to connect and support each other in new ways, and perhaps even empower people to reconvene, determined to take some form of action.
But these things don’t happen unless one makes them happen. There are those who are afraid of rocking the boat and confronting the powers-that-be. However, it is that very fear combined with the overpowering sense of despair and trappedness that sets the stage for suicide. We must understand that there is no one who is going to take care of us and look after our needs except us.
I also believe that the sooner we take such a proactive stance, there are many who will come forward as allies to join in that effort. Just as you Pamela have seen in your extraordinary efforts.
With deepest appreciation,
Kernan Manion, MD
Thanks Kernan. Great ideas. I hope others will join me in moving forward. We can’t sit on the sidelines any longer. Lives are on the line.
Maybe we should push for a policy, either through Joint Commission (or DNV), CMS, or even federal law, that a root cause analysis be performed whenever a physician suicide occurs. This would only apply to health systems, medical schools, and medical groups. The reports would need to be shared with appropriate authorities and sent to a central database. For solo or small group private physicians, this might have to be delegated to local law enforcement, but typically they don’t have resources, nor sufficient expertise, in performaing a true RCA. An RCA is what is done in the hospital setting for a patient suicide or other unexpected outcome.
Can you begin the process? We don’t have time to wait. This is an emergent situation and lives are on the line daily.
If doctors don’t want to get blamed for anything, then they do need to organize and have a union. They need to think that just because they are smart and highly educated, that they will get respect from these HMO CEOs. Nowadays, CEOs look at anyone n as an expendable, no matter how highly educated and skilled a person is Other groups have unions; however, that doesn’t mean that CEOs respect them as a matter of fact, the CEOs spend a lot of time to get rid of unions or fight against unionization.
Unfortunately, doctors are not legally allowed to unionize. They’re allowed to sacrifice their time, energy, and health caring for everyone else and suffer greatly in the process. Most physicians would not do it again nor encourage their children to practice medicine. It’s very sad.
Doctor can and do join unions. I’m a doctor and a member of the United University Professionals union.
That’s not true. Doctors can unionize. I’m a health care provider who is bargaining our first contract. We have MD’s, DO’s, NP’s, PA’s, Ph.Ds, LCSWs all in our bargaining unit. There are many doctors who are unionizing across the us. The only doctors who can’t are those who are in management.
I was trying to think what more could have been done before I turned to suicide which obviously was not accomplished. A comment stated the reason given was “she was troubled” . Yes by the time one turns to suicide you are “troubled”. Depression due to the overwhelming stressors of residency or practice then causes “troubles” in all other areas, ability to work efficiently because we physicians do keep working well up to the moment of suicide, relationships,care of your children,running of household, meals,cleaning, even care of my cat, financial, all aspects of your life. I had strong support from two fellow residents, my family practitioner PCP saw me weekly at the end of her day which helped but was not enough. I was on antidepressants. The missing ingredients were a therapist I trusted and support from residency administration. Hard to afford therapy if one seeks it self pay outside of insurance for secrecy or because the therapist or psychiatrist no longer accept insurance. After the fact (ICU admission) my residency admin was supportive. I had an attending advisor monitoring, another attending solely for support. And of course therapy was mandated. Admin told me their goal was for me to complete the residency program. I did go into debt for therapy and hospitalization as there was a cap on mental health coverage. Both the hospital and psychiatrist accepted small payments to my bill because I was a physician and with their help I would complete residency, and hopefully be able to pay all of my bill. No threat to losing my job. Residents need easily accessible Psychiatric care without stigma, without fear of losing job. I am not saying teaching programs dont need to change but if nothing else changes that alone can help.
Ali, It’s not easy for doctors to ask for help since we’re groomed in a culture that forces neglect of our bodily needs to hydrate, eat, sleep so that we can work inhumane hours. These suicides must be prevented. In each case there were 100s of missed opportunities to help the individual who was suffering. We simply do not often have the time or energy as residents and med students (struggling ourselves) to help others. There must be a recognition that the medical training environment causes or exacerbates ill health in doctors and we need more than lip service and reminders to meditate and sleep. I agree with your assessment and we absolutely need on-the-job accessible mental health care (if for nothing else the vicarious trauma of what we witness daily in a hospital). I’m so glad you survived and very sorry that you ended up in ICU before you got the care you needed. Your residency seems very supportive. What’s often missing is that culture of caring in which we can truly depend on one another. Like family.
A medical student once wrote me that she was less stressed in Afghanistan in an active war zone under sniper fire. Why? “The stress was incredible, but I had their back and they had mine. In an unsafe country and a future filled with uncertainty I felt secure because we supported each other.” https://www.idealmedicalcare.org/blog/medical-student-i-was-less-stressed-in-afghanistan/
I know it is not easy to reach out as ended up in ICU instead of reaching out when most needed to do so. I had compassionate residency directors and for that I am grateful. It did have a price. One of my favorite director attendings refused to give me a recommendation due to my mental health issues even though I recovered and did well my last year of residency. Good enough to work in hospital and clinics but not out in practice?
She could not separate the illness from my ability to now practice. I only want to let others know when reaching out to other doctors help them obtain psychiatric care as well as offer support. Go with them to that first appointment which one of my attendings did. Take their middle of the night phone call when they are on call. Support them. I had a list of 5 people I could call and that support was also key. We do have to take care of each other!
Hi, Ali. I’m a soon-to-be-former residency coordinator at an unrelated institution. First and foremost, you deserved nothing but utter support from your residency program: admin, PD, APD (if you have one–I don’t know), core faculty. And I am truly sorry that you didn’t receive the support you needed and deserved……before winding up in the ICU. My soon-to-be-former residents have my cell number to call at all times. And some have, particularly when feeling depression and dark cloud looming overhead. I’ve never regretted being available at all hours.
Residents’ fears of being stigmatized for seeking mental health or taking leaves of absence (for any reason) are very real. There wasn’t a single resident who met with me when we advised a leave of absence (LOA) who didn’t fear professional repercussions from potential future employers, board-certification entities (think ABIM), state licensing boards if their trainings were extended. It’s a disgusting state of affairs. This is no lie: in a boilerplate sample program manual our home institution distributes to programs each year, the LOA verbiage clearly states that taking a LOA is “burdensome to the program”, which is absolutely disgusting and ultimately untrue. A healthy resident is what a residency training program should strive to create.
All of this is to say that even if a program sufficiently supports its individual residents, the program has to swim against the currents of its own home institution (aforementioned wording example), ACGME (duty hours, lack of truly fostering competency-based residency curriculum/structure that gives residents greater flexibility in training), board-certification entities, to make this happen.
I wish you all the best in future practice, and your career.
Thanks for the insight and for going to bat to support residents. Eternally grateful for your example of compassion.
I don’t understand why the cops call suicides “no foul play.” Of course it’s foul play and yes there’s always a perp! I am a survivor of a mental health treatment-induced suicide attempt. I know I am not alone. Following incarceration in a mental hospital, chances of suicide multiply 100-fold, FOR THE NEXT YEAR. This statistic comes from a JAMA study. The AMA was embarrassed to publish this one. They wonder what the heck is wrong with the system! Look no further.
For one thing, these institutions need to stop wasting their efforts accusing people of suicidality who are NOT suicidal and should stop forcing treatment on people who don’t want it nor need it. This is a waste and it’s fraud. Force harms people and traumatizes them. And for those who want it, how about the right kind, the kind they actually ask for?
Thanks Pamela.
Forced hospitalization would not have been helpful if was not the treatment needed. Mandated therapy with therapist of your choice for the treatment you need a better approach. I dont know why hospitalization was mandated for you but I know if was not my choice to go in it would be hard to benefit from hospitalization.
I’m not so sure of the ethics of “forced therapy.” To legally force someone into treatment, there should be a high certainty of treatment success. Therapy patients who don’t want to be there, who are in a therapist’s office through coercion, are not likely to experience a good outcome. Maybe we all watched Good Will Hunting too many times.
It takes very little to trigger an Involuntary Psych Hold (usually 72 hours, some 5 days).A friend, spouse,family member can call 911 who must check out the situation and often take the person to the hospital where they are often held against their will and drugged. VERY coercive. And, as Julie stated, suicides are very common upon discharge. Serotonin drugs are documented to trigger suicidality during initiation of therapy, dosage changes, cold switches, and even after VERY careful tapering (advised at no greater than 10%/month decrement).
When prescribers make any changes, even switching to a different form of the same drug, it can trigger horrible withdrawal that is FAR worse than the original condition, but is usually misdiagnosed as a relapse or new condition.
The drugs are very powerful and increase serotonin, a HORMONE throughout the body, not unlike corticosteroids or estrogen.
This makes me so sad. I read the posts you listed, and I have a question. Many questions, actually, but one that haunts me is why the medical education system is so inhumane, so harsh. Does the establishment really think the methodology of creating dispassionate, sleep-deprived people is the best way to treat the sick? Or is it just because “it’s always been done that way”? I, personally, speaking as a patient, want my doctor to be human, compassionate, and well-rested. And, as a patient, how can I make a difference. I’ve read the list, but is there someone to write to? I have no friends or family who are doctors or medical students (though several nurses)? How is my voice made relevant?
1) Why medical education system is so inhumane? The patriarchal reductionist medical model (the basis of Western meded) is dehumanizing by nature. Add more expensive technology & higher throughput with no emotional support and it is a mental health catastrophe for medical students and physicians who sadly are too often valued primarily for their revenue generating capacity per second.
2) As a patient, how can I make a difference? By simple talking about these suicides. Please share the Do No Harm documentary film trailer (and see film when it debuts this year). Also read Kernan Manion’s comment on this blog as he has outline how you might proceed in demanding an investigation in these suicides. You should always ask your doctor how long he/she has been on shift and you have the right to request a doctor who is not sleep deprived. Your voice matters. use it.
Thank you for caring.
In part it is the regulations. Too many nonsensical regulations. Here. You have provided excellent care now jump through 20 hoops and document your care in 10 different places or else you/your hospital won’t get paid and you may be charged with fraud. Doctors need to determine what is reasonable documentation not administrators!
We’ve replaced common sense with CYA.
I also wonder how regulations and bureaucracy affect young doctors and their relationship to “burn-out” so early in doctors’ careers. Interns and residents have historically worked insane hours but suicide rarely happened. Along with the numbers game that regulation and bureaucracy require of doctors, technology has sped things up so much that there doesn’t seem to be much time to think and ponder. My late husband retired from medicine seven years ago after 50 years of practice and, while he loved technology and used it, he said that medicine wasn’t an art anymore, that doctors were becoming technicians.
Yes. The soul of medicine has been sold off. However, the next gen of doctors WILL take back the reigns and I have high hopes that we are starting to turn the tide on this fear-driven, patriarchal, reductionist medical system that has lost its heart and soul.
I, too, am am a resident doctor in NYC and while I feel I have a great support system within my program, the protection other healthcare providers (nurses, techs, etc) have is one I envy and it is expected we pick up their slack while managing 20 patients and trying to learn. Something needs to be done to help doctors in a city that needs us.
Absolutely. Please share any ideas you have. Urgent need to move forward now before any more lives are lost.
I think what Pamela is doing is great and very helpful, however the issue is still unfortunately largely unknown outside of the medical profession. In my opinion, the vast majority of readers of these types of articles are other medical professionals. The public at large do not know or understand how the medicine life works at all. The news that they do read/hear about are the misleading salaries of doctors because those are the type of articles that show up on mainstream news like Forbes, Yahoo.com, Bloomberg, etc. I cannot tell you how often people think I’m rich when they find I’m a doctor when in fact I am drowning in loans. I believe nothing will change and doctors/medical students will keep dying until the public is aware and demands change.
Things will soon change with the forthcoming film: Do No Harm: Exposing the Hippocratic Hoax. The public will soon understand that we are all in this together and can’t afford to sweep the truth under the rug one more day. All of our lives are on the line when our doctors are unwell. We must display the same compassion toward them as we expect to receive from them. Doctors are human.
Dear Pamela,
I so wish there was some simple answer to this needless, (yet for some reason, thought to be needed) behavior.
Is it the strain,… the years of endless shifts with bad food and no sleep? Is it the lack of OR the knowledge that FATHER has warned of, regarding the evil growing in these, the last days of this, the last generation? Is it the need for relationships that a physicians schedule don’t accommodate?
Is it the patient’s causing this somehow? Are their needs to seemingly entitled, asking for more than one should? Is it the opiod epidemic, with so many lives ending in their youth, setting up these doctors to see so many dying while not elderly,… but young, … still beautiful, and of their own ages?
IS IT THE FACT THAT THE NUMBER OF AMERICAN’S WHO ARE SICKLY HAS SUDDENLY SPIKED, due to a lobbyist-driven crusade to squeak a nickel out of even the lowest form of new genetically modified “food” manufacturers?
IS IT THE STRAIN OF ALL OF THE RETIRED, DECENT DOCTORS, who were once there for these up and coming medical giants? Or possibly the fact that the medical system in our nation has turned into the business of profit, and NOT the business of life saving?
Is it all of the above?
It’s funny (not haha either), that the patients today feel an equal push on their care, as they (we) see this strain as well!
Our doctors seem one of two things:
Either they are completely wonderful, full of fabulous energy that calms the entire situation (which perhaps was once thought too dire to even think on),… and their seeming endless joy seems to just spread among all involved in your care that day…Not only do these docs seem to have eaten their wheaties, slept 12 hrs the night before, but have such a true compassion for you that you’d swear they didn’t do this in a regular basis
OR
They’re simply complete arse’s, with no patience whatsoever, they’re rude, unwilling to help anyone, seem so frazzled and confused themselves, and it’s as if they’re not truly built for the job that they have now sunken their entire life into!!!
It’s as if they awoke one day to find they’ve been given a death sentence!!! The constant complaining of patients (because no one is happy being ill or in pain), so everyone you are going to see is going to be crying TO YOU for help! And WHAT IF those people end up OD’ing on a script you wrote?
There has to be a way to deal with ALL OF THAT, without punishing the truly ill,… those truly in pain!!!
And with the food supply being so toxic today, folks are becoming painfully ill with diseases that are often so hard to even diagnose… so THERE’S THAT!!!
There is too much stress on our doctors, for the amount of sick folks today!
If these diet-caused illnesses are spiking ( as they’re said to of), and 1 in 4 American’s are suffering truly painful conditions, then our doctors need backup and BAD!!!
If the patient numbers have doubled, why not the number of standing physicians????
Makes perfect sense to me!!! You can’t have a constant running number of very sick, HARD TO TREAT, COMPLEX, & MOANING folks constantly flooding in, TOPPED BY THOSE NEW STREET PUNKS, messing with your head about whether or not you should risk believing them about a sprained ankle or not,…. ALL with no break!!!
AND THEN GO HOME, half dead, starving for nutrition but giving in to whatever you can get your hands on while having to toss in a load of clean skivvies and brushing your teeth, after ALREADY having to somehow of found the strength to scrape the snow off your car, stop at the store, get gas, order new shoes on Amazon (cause yours are LEGALLY TOXIC now, and to then lay in bed, trying to relax, while paying the bills!!!
And the bills are now so horridly huge from this wonderful career now!!!! The fancy job that so impresses everyone (Everyone that you never have an opportunity to see, that is)…
A college bill totaling [at the VERY least] $150k, all for making this GLAMOUR JOB career move, …one that one doesn’t merely walk away from, once they’ve gotten through the door!!!
YEAH— IT IS STRESS—BIG TIME!
I do feel so badly for them all, but especially this new generation of docs, who have been given this extreme job, and have been left with stock holders on one hand, and nurses in the other (many foreign born now), and the stakes are higher than ever before…
THEY TRY TO MAKE IT TO PRIVATE PRACTICE, BUT THAT IS A LONG WAY AWAY… if you live through it…
that’s how I see it, anyway… after many conversations with the dozens and dozens of doctors I saw, while trying to be diagnosed with Pancreatic disease! I’ve spent a year and a half hitting up ER’s DAILY, as I begged and pleaded for help,… all over this nation.
And then, spent another 5 years traveling to at least a dozen out-of-state hospitals, to see specialists, once diagnosed.
I’ve heard and seen it all… I’ve been hugged AND cussed at, with not one bit of difference in my behavior or claims!!!
You truly have to put on your Big Girl panties to be able to hold a 2 minute consult with some of these folks, who are literally holding the reins on your getting care (or NOT)!!!
Most times, the tears I shed were caused from the cruelty I experienced, AND NOT MY KILLER PAIN!!!
There’s definitely something wrong with that picture…
and “I” am a VERY COMPASSIONATE PATIENT, when it comes to understanding their plight…….. You cannot have a more sympathetic patient than I am!!!
So, what do we do to help them? I know as a patient of this incurable disease, I have dove in deeply to our FATHER’S word… FOR WE ARE THE LAST GENERATION (per The Parable of The Fig Tree/Israel becoming a nation in 1948, and this now (2018) being that all-important “70 YEAR MARK”… FATHER WARNS US THAT THEY WILL BE HARS TIMES AND MAN’S HEART WILL FAIL FROM IT!!!
Is this suicidal crisis this “hearts failing”… ???
I would hope that they have HIM in their most inner being… Able to call on HIM, as HE is the COMFORTER!!!
Although, knowing what my Daughter experienced with a Masters Degree, and then her career,… there never seems to be any time for learning even the most basic of what we MUST know… what HE instructs us to know…
I would say, more help is needed!
Less profits needed!
More down time and NO OVERTIME for those in this field… it is simply INHUMANE and EXTREMELY RISKY for the doctors to be treating life and death… YEP,… LIFE….. DEATH… with little to no sleep!!!!!!!!
The fact that this has been going on for so long just blows the mind!
It is the most urgent of all of the issues I see in the medical INDUSTRY!!!
FOR HEAVEN’S SAKE,…. LET THEM REST!!!!!!!!!!!!
Sincerely, Carolyn Nunes
This is horrible! And facebook wiped it so I am going through the back door. Not what I originally wrote because it was “reloaded.” That was shorter and more concise, but the message is the same.
Where suicide is concerned I cannot believe the medical community still stands in the grip of the attitudes of the 19 and 20th centuries. In war this sort of thing was labeled “lack of moral fiber.”
I am the daughter of a 1961 sucide. My father was a musician. I still remember everything. The shock, the grief, the anger, the guilt, the bewilderment because no one told us children anything ever. I remember being instructed by various family members to say nothing to anyone. I remember returning to 4th grade class the next day and being looked at. I remember the adult faces telling me that if I was asked they should consult my grief stricken mother. I STILL know NOTHING and am 66! I had to live my life making up reasons. He was depressed is all I have. This society has left generations of the children and families of suicides confused, in despair, and walking the world like wraiths, never quite connected with anyone. There should be openness, not shame. I am so angry at this report. No one is helping the survivors, let alone the abused medical students. And there are other professions that do the same. There should be research, the results published. Open forums. Places where burnt out but valued individuals can go without fear of shame, get help, and then return to their training and their jobs. I am SICK of THIS attitude! It is your country, your neighbor, your friend, your society. This has to change. All these resources, being people with talents, personalities and minds are lost forever.
I’ve spoken to others who have experienced a lifetime of confusion and unprocessed grief due to this ongoing suicide censorship. We really do need to release our souls from the grips of the dark ages when it comes to our mental health.
I am so sorry for this doctor…. Why, because that broken, lifeless body underneath the tarp could very easily have been me. I think we docs need to walk w our feet, and stop practicing medicine, even if our next job might be burger flipping or housecleaning or babysitting. Just about any other job is better than being a slave on the medical factory assembly line. If you are a medical student, minimize your debt,and try to get out while you still can. It is a decision that may save your life!
Or best of all . . . open your own practice if you can. No need to be pinned under so much infrastructure for most outpatient medicine practices. Liberate yourself. Here’s how: Don’t let your job suck your life out of you.
I too worked in the medical field but not as a doctor but as a psychiatric technician in a NYC hospital and due to a patients false allegation I was terminated after being cleared from the hospital of wrongdoing this situation has put me in a severe depression which at times I consider suicide because of losing my Home my car my job. We as medical professionals have no rights when it comes to false allegations by patients we work hard going to school taking our loans to be in a profession that we love and can be taking away in a heartbeat so some of professional feel this is the way out
Doctors job is demanding physicall and mentally .doctors suppose to cure other so they should cure themselves first.working in groups ,share their problems together because no one knows their problems issues than themselves. Also they should have astrong relationship with God. Putting in mind killing yourself is against god willing we are the ones giving life to other,so better to give to ourselves.
Thank
What do the school systems do when there is a suicide at school. Counsel them. No one is excluded from feelings. Doctors are not superficial. We all are born, live life, and we all die. End of story. They are not immune to tragic. We all process things differently. I am not a doctor but praise them wrong or right. Someone has to help the helpless and when you save someone (1) person it is the best feeling. Talk about it, cry about it, hug about it, but Not talk about it will fester until you break. Bless you all for all you do. You can’t save everyone, but all you can do is try and that is all we can ask for. They should have a meeting three times a week for an hour to vent. Have someone talk with someone who knows how the Union works and go from there. There should be repercussions of bullying if that is what is going on. Someone claiming they are not doing enough, it is teamwork!! Learn from a lesson not to be demeaned is not the right way to go about correcting the problem. I am sure whoever is in charge, was not born with all the answers. Pray for all involved and sorry for the loss of all the beautiful doctor (s).
If you are a physician at Mt. Sinai St. Luke’s and have a story you would like to tell about how the hospital handles staff suicides, please contact me.
I am so sorry for your loss.
I am a professional patient, with over 15 diagnosis’. I have a lot of caring, amazing doctors who help me over and over. I have however, asked myself how a hospital would allow residents to work shifts that no mere mortal could accomplish! Do they think about the toll the slavish hours take on doctors? The amount of errors that could be reduced by allowing a human being to get enough sleep, enough rest to care properly for their patients? Doctors committing suicide due to both physical and mental exhaustion, due to not feeling adequate enough? Come on now insurers and hospital top brass! This HAS to change!!! Respect and honor these docs that work their tuchas off and are committed to helping all patients…RIP doctors that could have made a difference in someone’s life,maybe even mine.
We in the nursing profession are also blamed constantly for what others do, BUT we tend to have each other. We also have a union that we can rely on if need be, who do the doctors have??? I have talked about this suicide cases with others and what I hear is “there has to be somthing else she was going through”. why can’t it be that the mental demand of the job and lack of empathy in the medical field for the medical profession is very poor. I know back in the days lot more was expected of them as interns used to work over 100 hrs a week. We have to put in perspective that soooooo many don’t have families, friends in their new towns,cities , countries. Away from home, following a dream that maybe was not their dream , but their families. We need to educate ourselves and remind each other WE ARE HUMAN, that the human in us needs love, hugs,empathy,smiles, food, water.
love that you are raising more attention to this huge secret in the medical profession …. DEPRESSION IS REAL AND NOT SHAMEFUL
So very sad.
It appears our primary sources for and who render compassion and healing cannot find the very same when they also need it.
Thank you healthcare professionals for all you do every day!
“There is no silence as profound as that which greets the news of a suicide in the medical community.” ~ M.J. Legato
“Physician suicide is seldom mentioned in the electronic media, and scant mention is made of it in print. A newspaper publishes a suicide note from time to time, but this is rare.” M. Desjardins
12/26/1886 Archives. A Physician’s Suicide: Dr. Henry Andrews, a physician who has boarded at the residence of Mrs. George L. Knight, at 569 Grand Avenue, Brooklyn, for the last two years, committed suicide about 2 o’clock yesterday morning by shooting himself . . .
A student at our school died by suicide. I don’t think everyone knows this, since the school has been vague when addressing it as a group. I find this response from a faculty member in the department of ethics to be worrisome. But it highlights what I’ve seen from our school. It suggests to me that this is par for the course, and that we can do nothing to prevent this from happening.
After a student dies, I think an objective committee should review what happened, and that team should include faculty and experts from outside of the school. And there should always be an objective liaison for students to reach out without fear of retaliation. We would expect this for a patient’s death in the same manner, so why wouldn’t we do this for a colleague?
Have you noted any pattern at certain institutions? I started residency in California. I ended up at Mt. Sinai in NYC. It was like night and day. While my previous program was supportive and nurturimg during one of the hardest parts or our careers—sinai was horrible. The environment is so cold and harsh and cut throat. It was so bad that a number of the cheif residents had to be talked in to going to the graduation so the dept wouldn’t look bad. I found out why when i myself felt humiliated when I graduated and the dinner celebration where my family and friends had come across the country for graduation only to have a gruesome “roast” of the cheifs. Residents are routinely criticized and not supported and subtly encouraged to lie about our work hours. I was actually not surprised to hear of a couple of suicides out of Sinai a couple years ago. I was warned it was a “malignant” program and it was. Having had the benefit of a non malignant program i had already had my confidence built up and supported and i knew that was not normal or right- unfortunately most of the other residents had no comparison – so accepted that as normal. I’ve never said anything about this so please do not share my name—but keep an eye on malignant programs that push stressed residents over the edge.
A piece is missing here and I often think about how abuse rolls down onto patients. I’ve spent half my “career” as a doctor and half my “career” as a chronically ill patient. I have come to despise physicians as a group. Even as a patient, once they know I’m a physician it’s an invitation for abuse. Almost everywhere, it seems the patient is the enemy. Hospitals get more slick about covering up physician and nursing wrongdoing and their fancy electronic records hide many sins through the fabrication and falsification of records. I’ve seen and personally experienced plenty of patient abuse. The last hospital I was at after getting hit by a car had an atmosphere of toxic masculinity and “the boys” roamed the halls like cowboys, accountable to no one. Where were the attendings? Freewheeling it. I tell people to never go into a big corporate hospital alone—it’s not safe.
Yes this is a legitimate abuse cycle. What was once a healing profession has devolved with the invasion of third parties and many other complex factors. Including lack of confidential mental health care for doctors who are victims of vicarious trauma (by the nature of their very work).