
Article featured in The Washington Post and Chicago Tribune.
Five years ago today I was at a memorial. Another suicide. Our third doctor in 18 months.
Everyone kept whispering, “Why?”
I was determined to find out.
So I started counting dead doctors. I left the service with a list of 10. Five years later (10/28/17) I have 547.
[As of 9/17/21 there are 1,710 doctor suicides on the registry. If you’ve lost a doctor or medical student to suicide, please (confidentially) submit names here.]
Immediately, I began writing and speaking about suicide. So many distressed doctors (and med students) wrote and phoned me. Soon I was running a de facto international suicide hotline from my home. To date, I’ve spoken to thousands of suicidal doctors; published a book of their suicide letters (free audiobook); attended more funerals; interviewed surviving physicians, families, and friends. I’ve spent nearly every waking moment over the past five years on a personal quest for the truth of “Why.” Here are 35 things I’ve discovered from the first 547 cases:

High doctor suicide rates have been reported since 1858. Yet more than 150 years later the root causes of these suicides remain unaddressed.
Physician suicide is a public health crisis. One million Americans lose their doctors to suicide each year.
Most doctors have lost a colleague to suicide. Some have lost up to eight during their career—with no opportunity to grieve.
We lose way more men than women. For every woman who dies by suicide in medicine, we lose four men. (amended 3/7/19)
Suicide methods vary by region and gender. Women prefer to overdose and men choose firearms. Gunshot wounds prevail out West. Jumping is popular in New York City. In India doctors are found hanging from ceiling fans.
Male anesthesiologists are at highest risk. Most die by overdose. Many are found dead in hospital call rooms.
Lots of doctors die in hospitals. Doctors jump from hospital windows or rooftops. They shoot or stab themselves in hospital parking lots. They’re found hanging in hospital chapels. Physicians often choose to die where they’ve been wounded.
“Happy” doctors die by suicide. Many doctors who die by suicide are the happiest most well-adjusted people on the outside. Just back from Disneyland, just bought tickets for a family cruise, just gave a thumbs up to the team after a successful surgery—and hours later they shoot themselves in the head. Doctors are masters of disguise. Even fun-loving happy docs who crack jokes and make patients smile all day may be suffering in silence. We are all at risk.
Doctors’ family members are at high risk of suicide. By the same method. One physician died using the same gun his son used to kill himself. Kaitlyn Elkins, a star third-year medical student, chose suicide by helium inhalation. One year later her mother Rhonda died by the same method. At Rhonda’s funeral, I asked her husband if he thought his wife and daughter would still be alive had Kaitlyn not pursued medicine. He replied, “Yes. Medical school has killed half my family.”
Suicidal doctors are rarely homicidal. Of the first 547 suicides I’ve compiled, only 2% (15) involve homicide. Half (7) are male physicians who killed a female spouse/girlfriend (all in health care—4 nurses, a nursing student, pharmacy tech, and dentist). Three male physicians murdered their young children. Another strangled his disabled adult daughter before killing himself. Less than 1% of all doctor suicides involve homicide of their children. Here’s why surgeon Dr. Chris Dawson shot his kids before turning the gun on himself. Of the 3 cases involving young children, all suicide victims were having marital/relationship problems with the mother. One also killed the mother.
Doctors have personal problems—like everyone else. We get divorced, have custody battles, infidelity, disabled children, deaths in our families. Working 100+ hours per week immersed in our patients’ pain, we’ve got no time to deal with our own pain. (Spending so much time at work actually leads to divorce and completely dysfunctional personal lives).
Patient deaths hurt doctors. A lot. Even when there’s no medical error, doctors may never forgive themselves for losing a patient. Suicide is the ultimate self-punishment.
Malpractice suits kill doctors. Humans make mistakes. Yet when doctors make mistakes, they’re publicly shamed in court on TV, and in newspapers (that live online forever). We continue to suffer the agony of harming someone else—unintentionally—for the rest of our lives.
Doctors who do illegal things kill themselves. Medicare fraud, sex with a patient, DUIs may lead to loss of medical license, prison time, and suicide.
Academic distress kills medical students’ dreams. Failing boards exams and being unmatched into a specialty of choice has led to suicides.
Doctors without residencies may die by suicide. Dr. Robert Chu, unmatched to residency, wrote a letter to medical officials and government leaders calling out the flawed system that undermined his career prior to his suicide.
Assembly-line medicine kills doctors. Brilliant, compassionate people can’t care for complex patients in 10-minute slots. When punished or fired for “inefficiency” or “low productivity” doctors may choose suicide. Pressure from insurance companies and government mandates further crush the souls of these talented people who just want to help their patients. Many doctors cite inhumane working conditions in their suicide notes.
Bullying, hazing, and sleep deprivation increase suicide risk. Medical training is rampant with human rights violations illegal in all other industries.
Sleep deprivation is a (deadly) torture technique. Physicians have suffered hallucinations, life-threatening seizures, depression, and suicide solely related to sleep deprivation. Sleep-deprived doctors disclose hospital horrors that kill or injure patients. Others die in fatigue-related car crashes after long shifts. Resident physicians are now “capped” at 28-hour shifts and 80-hour weeks. If they “violate” work hours (by caring for patients) they are forced to lie on their time cards or be written up as “inefficient” and sent to a psychiatrist for stimulant medications. Some doctors kill themselves for fear of harming a patient from extreme sleep deprivation.
Blaming doctors increases suicides. Words like “burnout” and “resilience” are often employed by medical institutions as psychological warfare to blame and shame doctors while deflecting attention from inhumane working conditions. When doctors are punished for occupationally induced mental health conditions (while underlying human rights violations are not addressed), they become even more hopeless and desperate.
Sweet, sensitive souls are at highest risk. Some of the most caring, compassionate, and intelligent doctors choose suicide rather than continuing to work in such callous, uncaring and ruthlessly greedy medical corporations.
Doctors can’t get confidential mental health care. So they drive out of town, pay cash, and use fake names to hide from state medical boards, hospitals, and insurance plans that ask doctors about their mental health care and may then exclude them from state licensure, hospital privileges, and health plan participation. (Even if confidential care were available, physicians have little time to access care when working 80-100+ hours per week).
Doctors have trouble caring for doctors. Doctors treat physician patients differently by downplaying psychiatric issues to protect physicians from medical board mental health investigations. Untreated mental health conditions may lead to suicide.
Medical board investigations increase suicide risk. One doctor hanged himself from a tree outside the Florida medical board office after being denied his license. He was told to “come back in a year and we will reinstate your license.” Meanwhile he lost everything and was living in a halfway house.
Physician Health Programs (PHPs) may increase suicide risk. Forcing doctors with occupationally induced mental health issues into these 12-step programs with witnessed random urine drug screens (when they’ve never had a drug problem!) is humiliating and unethical. So doctors hide their mental health conditions for fear of being punished by PHPs. [Note: PHPs have helped some doctors with substance abuse especially]
Substance abuse is a late-stage effect of lack of mental health care. Since doctors may lose their license for seeking mental health care or get locked into PHPs; they self-medicate with alcohol, illicit drugs, or self-prescribe psychotropic medications.
Doctors develop on-the-job PTSD. Especially true in emergency medicine. Then one day they “snap” like this guy.
Cultural taboos reinforce secrecy. Suicide is a sin in many religions. Islam and Christian families have asked that I hide the suicides of family members. Indian families often claim a suicide is a homicide or an accident, even when it’s obviously self-inflicted.
Media offers incomplete coverage of suspicious deaths. Articles about doctors found dead in hospital call rooms claim “no foul play.” No follow-up stories.
Medical schools and hospitals lie (or omit the truth) to cover up suicides—even when media and family report cause of death. Medical student Ari Frosch stood in front of a train, yet his school reported he died at home with his family. Though the family of psychiatrist Christine Petrich shared that she bought a gun and killed herself (after just getting her hair done and planning a surprise trip to Lego Land and Disney for her kids) on their GoFundMe page, her employer wrote she “passed away.” Shouldn’t the department of psychiatry take a more active interest in physician suicide?
Euphemisms cover up doctor suicides. Suicide is omitted from obituaries, funerals, clinics, hospitals, and medical schools. Instead we hear “passed away unexpectedly in her sleep” and “he went to be with the Lord.”
Secrets will not save us. We’re unlikely to make a medical breakthrough on a hidden medical condition.
Doctors choose suicide to end their pain (not because they want to die). Suicide is preventable. We can help doctors who are suffering if we stop with all the secrecy and punishment.
I’ve been shunned for speaking about doctor suicide. After being invited by the AMA to deliver my TEDMED talk, I was disinvited shortly before the event because they were “uncomfortable” with physician suicide.
Ignoring doctor suicides leads to more doctor suicides. Thankfully, an Emmy-winning filmmaker is completing a documentary on physician suicide this year. To honor a doctor or medical student who has died by suicide in the film, submit name here. Contact filmmaker for a screening at your medical school or hospital.
If you are currently suffering and need help, contact Dr. Wible. Monthly physician retreats ongoing. Have you lost a medical student or doctor in your family to suicide? Request to join our Facebook support group here.
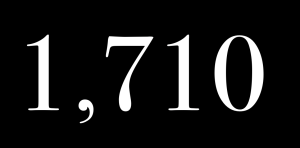












I worked 216 hours in the last 2 weeks. Slept 17 hours in the last 1 week. I’m exhausted. No hope for change anytime soon.
Wait until you see the film and patients FINALLY understand the dangers of sleep deprivation and human rights violations in medicine that trickle down onto everyone. Did you see the film trailer? http://donoharmfilm.com
Very sad. There are no regulations limiting the hours attending physicians can work. Without collaborative agreements between hospitals and private practices for covering call we are creating dangerous/abusive situations. The problem is hospitals are often not willing to work with private physicians leaving no options as we can not abandon our patients ethically or by law. It’s a lose-lose.
We have the resourcefulness and native intelligence to solve this if we stop hiding the truth in the shadows. We all deserve to know the truth of the working conditions in hospitals and clinics.
Connie,
Perhaps you are in training. But if you have finished your training there is a better way. Certainly Pamela can give you ideas. I am also working on a project to change the equation for idealistic doctors trying to work for their patients, families, and communities. Colleagues like Pamela and I can help.
i did send the correct email address.
Doctors are human. A fact many do not understand including doctors. We all need good support systems especially at home. We need God in our lives too.
It is the toxic work and cultural environment, not the lack of resilience or strength of the individual. Tell it, Dr. Wible!
From my blog Burnout is a smokescreen for human rights abuse:
“Burnout” is a smokescreen for rampant human rights violations in medicine. Am I losing anyone here? Let me break it down.
“Burnout” is a complete mental and physical collapse from overwork. Psychiatrists define it as a job-related dysphoria in an individual without major psychopathy. Which means—your job sucks. You’re normal
Smokescreen is an artificial cloud of smoke that hides the perpetrator’s true intentions. This cloud of smoke may take the form of a statement or word used to obscure the truth so victims don’t understand what the heck is really going on. For example, apply the victim-blaming term “burnout” to deflect attention from oppressors who are guilty of human rights violations.
Human rights violation is the violation of a basic right to which all humans are entitled, including the right to life, liberty, equality, a fair trial, freedom from slavery and torture, and freedom of thought and expression. Common human rights violations in medicine include: 1) Sleep deprivation (24+hour shifts, 80+hour work weeks) as described by this physician whistleblower who was forced to work 168-hour shifts. 2) Not being allowed to eat, poop, pee when one needs to 3) Bullying and hazing 4) Being terminated, harassed, or threatened rather than receiving accommodations under the ADA for mental or physical health issues as described by this physician whistleblower who nearly died when her hospital obstructed her medical care.
Physician whistleblower is a physician who reveals health care’s human rights violations to the public. If you’re a physician with a whistleblower story, contact me. Doctors must stop being complicit with abuse or they will become the perpetrators (see below). Physician whistleblowers protect themselves, other health professionals, and patients from continued abuse. Silence and secrets protect the perpetrators.
Victim is a person harmed, injured, or subjected to oppression or mistreatment (may include being sacrificed or killed due to an action/inaction). Those who don’t know they are victims are at high risk of becoming perpetrators.
Perpetrator is an individual (acting alone or within a system such as a medical school, residency or hospital) who harms, injures, or subjects another to oppression or mistreatment (may include sacrificing or killing someone else due to perpetrator’s action/inaction).
Burnout is a smokescreen for rampant human rights violations in medicine. One way to end a cycle of abuse is to stop blaming the victims. Tell the truth: it’s not burnout, it’s abuse.
“rampant human rights violations in medicine” is an understatement!!
Every citizen in the United States, physicians, and patients have been tricked, betrayed, deceived, confused, miseducated, and paid not to care or think for themselves. Especially to figure out what happened to THE MOST ethical, moral, and honorable profession., A Physician.
[remainder edited by moderator as off topic]
this is a thinly veiled diatribe and very off topic. It should be removed, or edited perhaps down to the first line.
Hate censorship though you are correct. Will be limiting to first graph now.
Dear Pamela, I didn’t know that the AMA put their heads in the sand. Aren’t they there FOR their members? You know you are doing very important work, don’t you? So, keep going, keep talking about it, because it is REAL, AUTHENTIC, and for the sake of every doctor and their families is a story that MUST be told!
For the sake of all of us who will ever seek the care of a doctor.
Fantastic post, Pamela. Thank you.
Thank you, Pamela Wible for your tireless efforts to shine a light on the important subject!
I’m glad to see your article come to fruition. God bless all of them. I think it’s about time physicians learn to stand up for themselves…they NEED TO…they are beaten into the ground by lawyers, insurance companies, angry patients, and politicians. You have got to get organized or it’s going to get worse. Just this week it was announced that the opioid crisis in this country was due to over-prescribing! Well, when “PAIN” is made the 5th vital sign and it’s being driven by Medicare/Medicaid and then reimbursement is fueled by patient satisfaction and PRESS-GANEY scores, why is anyone surprised!?
Part of the problem is:
1) Doctors don’t understand that they have been victimized (or are unwilling to accept the extend of their victimization).
2) Most doctors seem to fall for the psychological warfare embedded in words like “burnout” and “resilience” and “work-life” balance which deflects attention from the perpetrators of these human rights abuses and make doctors feel defective for not being able to keep up with the inhumane requirements of their job.
3) Divide-and-conquer and intimidation tactics have worked well thus far to keep doctors pitted against each other instead of truly standing up for their own rights and the rights of their colleagues.
We have been wounded by medicine and resist grasping the extent of the wounds.
Suicide becomes one way to end the pain.
I can truly say this mass-wounding of our healers is one of the sickest things I have witnessed in my lifetime. Tragic beyond belief.
How much do you think that many of us who choose a career in medicine are wounded to begin with? David Zigmond gives a rare analysis of the paradox of the wounded physician.
In my experience of working with stressed GPs and trainee GPs, many of them have had to deny their emotional needs from a very early age, were made to feel that they were never good enough, that failure wasn’t an option and their goal in life was to attend to other people’s needs. We (doctors) are rarely encouraged to think about how experiences of care and being cared for led us to choose a medical career, or to reflect on our shame at being seen to be emotionally needy or vulnerable in the eyes of our peers.
None of this is to deny that the cultures in which we work are not toxic, but it does help to explain that on the whole, it’s doctors who have built these cultures
Yes. That savior complex stats early for many. We hope to heal others to in some way also heal ourselves. Many of us are driven to choose the profession based on personal suffering, witnessed abuse of others, traumatic events with family members (parent or sibling dying young of cancer). We need an educational environment that does not further torment those who choose the healing arts. We need (obviously) emotional support to do the amazing work we are capable of in medicine.
Dr Wible, I cannot describe how meaningful your work is. Thank you for exploring such delicate subject
Labor of love for my beautiful profession and so many true healers who were not able to give their fullest gifts of healing to the world. Many have been so tragically shunned in the deaths. Certainly a civilized society should honor and nurture its healers from a young age and celebrate them even after their deaths. I for one am unwilling to forget them. Thank you for caring so deeply Diane.
Dr. Wible, Please contact Megan Kelly for a show on this subject and bring this into the homes of America.
Sure! What’s her ph#? Feel free to suggest on my behalf if you know her.
I’m a Child, Adolescent and Adult Psychiatrist who is currently not providing clinical care in part related to some of the wear and tear that my chosen profession has added to my life. Luckily, I found other work that utilizes my skills. I’m not sure if I will return to clinical care. I have mixed feelings about this for lots of reasons, but especially because there aren’t enough us out there.
In my practice, I treated many depressed/suicidal MD’s including residents and fellows and it was very difficult, upsetting and rewarding. It is always tragic when someone chooses to end their life and even more tragic for those families with several members have made that choice
However your statement “I can truly say this mass-wounding of our healers is one of the sickest things I have witnessed in my lifetime. Tragic beyond belief.” is where you lost me. Child abuse/neglect that never ends despite having multiple systems involved for years. Domestic violence victims that aren’t believed/protected and eventually killed by their perpetrators no matter what they do or who they ask for help. A huge majority of runaways after 48 hours being tricked or kidnapped into sex slave trade.
And this is just in our very privileged country.
No, I have not personally witnessed all of these atrocities, just like I haven’t witnessed the horrors in Syria.
It’s just hard for me to get behind that sentiment despite losing colleagues/patients to suicide and applauding you for taking on this serious crisis.
“I can truly say this mass-wounding of our healers is one of the sickest things I have witnessed in my lifetime. Tragic beyond belief.” I think this statement comes from personally witnessing some of the most caring, compassionate, loving people of my life succumb to suicide over and over again at the hands of a “health care” system. I am not saying this is worse than other terrible crimes against humanity but it IS the worst thing I have personally witnessed in my life so far. I’m a very emotional person as you probably have figured out and it is hard for me to contain my absolute horror at what I have personally seen in (mostly men) doctors who I’ve loved go down one after the other. . . often for short-term greed (as declared in their suicide notes). It really is unbelievable.
“Just this week it was announced that the opioid crisis in this country was due to over-prescribing!”
Which seems to be a fact. Orthogonal to the issue of physician suicide, unless you really want to engage in whataboutism.
Deal with the most pressing issue first. The authors claims:
“I’ve been shunned for speaking about doctor suicide. After being invited by the AMA to deliver my TEDMED talk, I was disinvited shortly before the event because they were “uncomfortable” with physician suicide.”
That’s the most pressing issue. The people who shunned her for speaking about doctor suicide should be sued and locked in jail. It’s too serious an issue to indirectly condone shunning in this way.
I remember the first day of medical school, August 1991: introductory lecturers warned all of us doctors had an especially high risk of suicide and to guard against it.
The only time my entire life I became suicidal was during my residency in the mid-1990s. We were asked to track our work hours, record them, and turn them in. I, at least, was working 90-110 hour weeks, so the idea of adding another task to my plate was laughable, even though I realized had I done so, it might have meant an objective measure to effect change. I couldn’t have done it if I tried! I was far more focused on practicing how to sleep like a dolphin, where half my brain rested while the other still functioned! I somehow learned to take quick naps while standing upright during rounds or while taking a history from a patient or in the middle of dictating an intake history or discharge summary.
I was told, at the time, a first-year Internal Med resident had committed suicide by hanging himself in a call room during his first month of rotations. I also was told one of my former medical school classmates killed herself near the end of her anesthesia residency by hooking herself up to IV propofol in an empty patient room.
Welcome-to-medicine lectures are very scary. Here’s one I share in chapter 1 of Physician Suicide Letters—Answered:
Dear Pamela,
Thank you so much for the truths you speak for so many. Many times in my years of medicine I have said to trusted friends and to several therapists, “Something happened to me in med school.”
I was happy, secure, and mostly unafraid until med school. I recall in vivid detail the first orientation day. Our anatomy professor stood before an auditorium filled with 125 eager, nervous, idealistic would-be healers and said these words: “If you decide to commit suicide, do it right so you do not become a burden to society.” He then described in anatomical detail how to commit suicide.
I have often wondered how many auditoriums full of new students heard those words from him. I am sure someone stood in front of us and told us what a wonderful and rewarding profession we had chosen. I do not rememember those words. But I do remember how to successfully commit suicide—with a gun.
One month later, on the eve of our first monthly round of six exams in one day, I had my first full-blown panic attack. I had no idea what was happening. I thought I was losing my mind. I took a leave of absence and made up excuses. I returned untreated with maladaptive compulsive behavior, completed med school, survived the public “pimp sessions,” and all the rest.[Pimping is a “teaching” technique in which a student is grilled with rapid-fire questions (often about obscure medical minutiae). These much-feared public interrogation sessions can be so malicious that the student may be left crying—in front of peers, staff, and patients.]
No one ever suggested that the process was brutal, or the responsibility frightening, and no one offered us help. I have maintained contact with only one colleague from med school, so I do not know how the others fared.
Through the many years of training, and through what would appear to the observer a successful career in a surgical subspecialty and now into retirement, I have carried the anxiety, and the depression, and the fear. Perhaps entirely unrelated to those first days in med school, but still something happened to me, and probably to many of us, that changed us forever. I still remember how to successfully commit suicide, because someone who had power over me at a vulnerable time described the details. And we wonder why . . .
~ Anna
Download free audiobook here. Its like a 3-hour doctor suicide hotline call with me.
Regarding the issue of “happy doctors” dying I wish to quote from the 1858 book I referenced in the beginning of this blog:
“Carlini, a French actor of reputation, consulted a physician to whom he was unknown, on account of the attacks of profound melancholy to which he was subject. The doctor, among other things, recommended the diversion of the Italian comedy; “for,” said he, “your distemper must be rooted indeed, if the acting of the lively Carlini does not remove it.” “Alas!” ejaculated the miserable patient, “I am the very Carlini whom you recommend me to see; and, while I am capable of filling Paris with mirth and laughter, I am myself the dejected victim of melancholy and chagrin!”
Recalling the suicide of Robin Williams and many wounded healers every time I read this.
From: Bucknill JC, Tuke DH. A Manual of Psychological Medicine. London, England: John Churchill; 1858
My first attempt at writing this same blog 5 years ago. Very interesting list of 35 reasons doctors die by suicide (written by a novice Pamela)
“Physician Health Programs (PHPs) increase suicide risk. Forcing doctors with occupationally induced mental health issues into these 12-step programs with witnessed random urine drug screens (when they’ve never had a drug problem!) is humiliating and unethical. So doctors hide their mental health conditions for fear of being punished by PHPs.”
Do you have evidence of this?
I think that there is a correlation between the two but not a causal relationship.
Since these doctors are already mentality ill, their risk for suicide is already increased.
My suicide risk went down when my PHP intervened. They found me proper treatment. So my personal experience refutes your claim. PHPs help impaired physicians not hurt them!!!!
Thanks for sharing Marcus. Calling you now. I will return to a first draft of this entry where I had “may” inserted in there and will add an addendum indicating that there is wide variation from state to state.
Physician Health Programs (PHPs) may increase suicide risk. Forcing doctors with occupationally induced mental health issues into these 12-step programs with witnessed random urine drug screens (when they’ve never had a drug problem!) is humiliating and unethical. So doctors hide their mental health conditions for fear of being punished by PHPs. [Note: PHPs have helped some doctors with substance abuse especially]
An example of how PHPs have not been helpful (I have a section in Physician Suicide Letters—Answered devoted to PHPs):
Dear Pamela,
I’m amazed at the punitive terms I’ve had to face in recovering professionally from a depressive episode for which I was hospitalized last year. One of my requirements is to be urine tested for substance abuse, despite multiple demeaning assessments that have rendered the clear verdict that I don’t have a substance use problem. I’ve had to attend costly treatments for “professionals” in which I am the only female in a group of male physicians who have had sex with their patients or have become assaultive with staff. Any efforts on my part to point out that I don’t quite “fit” are taken as further evidence of my pathology. I’m a single parent as well, so that each of these “treatments” I’m required to attend takes me away from my two children for extended periods of time. throughout all of this, nobody has told me how common my feelings are—that a large number of doctors feel depressed and suicidal at times. Rather, I’ve been told that my actions are unheard of for someone in mental health and may preclude me from ever providing therapy again since “we tell patients to never give up hope, but you did.” Hopefully, in the near future this won’t be a taboo subject, and there will be places for those like me to seek responsible and con dential care.
Sincerely,
Amy
Yes, a key problem of PHPs according to my clients is that PHPs often have only round holes, such as twelve step programs, “preferred” physician assessment and rehabilitation centers that invariably diagnose significant illness and prescribe prolonged –cash only–inpatient stays and drug testing schemes, into which they try to stick “square clients” such as yourself to maximize their apparent efficiency and profits. Then, when the squared edges start to shear off, they label the victim a “denier” of sameness or accuse them of “substantive noncompliance”, or in the case of substance use “Level 1 relapse: behavior without chemical use that is suggestive of impending relapse”…terms the PHPs have cleverly had written into FSMB policy, to extend their ability to report such substantive “noncompliance” to medical boards and use the physician’s license to hold him/her hostage to their preferred methods. There are plenty of reports of this, and some will be explored in “Do No Harm”.
Marcus, so glad that the system worked for you. Perhaps you are “round”. Please do not assume that your experience is perfectly typical.
PHPs vary greatly state to state. I am currently conducting a confidential survey on state PHPs and your input would be very helpful (link below). Although you had a positive personal experience with your state PHP many others have had very negative experiences. Not all of those referred to or being monitored by PHPs are “already mentally ill” and many do not even meet the diagnostic criteria for Substance Use Disorder or psychiatric diagnoses for which they are being monitored ( substantiated by second, third and fourth opinions from experts). Complaints of financial exploitation and “diagnosis rigging” are increasingly coming to light. To assure organizational justice oversight, regulation and some form of accountability is needed.
Full exploration and investigation would be most helpful. Great variation state by state.
Maybe for you, but you can’t speak for all of us. I was diagnosed w reiter’s and tried numerous modalities without success. I had pain and I made a mistake and took a cortico-steroid out (and used the patient’s name–which made it diversion). I admitted my fault but also told the rehab facility I had chronic pain and was seeing ortho to manage my issues. I have never abused medicaiton however they found I was bipolar and a steroid addict.
It’s funny because the DSM 4 does not recognize a steroid addiction. Plus I could control my use of the medicaion. I just was having a lot of pain one day and I needed an injection into my foot. And that’s all she wrote. My program fired me. I went to a 3d eval bc they reported the diversion and then after being labeled an addict and having NOT finished a residency, I have been unhireable. So tell me again how these shit bags help anyone. If you were there because you wanted to be there, then congrats, your willpower helped you thru as well as having gainful employment available when you were done.
I had my car repod, my wife left me, I lost my job, I was branded an addict, I was unemployable, I couldn’t get into a residency because everyone treated me as though I was an addict. And I struggled to find money to pay rent so if you didn’t suffer that and you were able to get your life back on track, then don’t pretend to know what people go thru and the suffering they experience. I’ve had more suicidal thoughts than you can imagine. I’m up everynite relieving my past and feeling ashamed and worthless. Welcome to the justice system of the US. Designed to humiliate you, scar you, make your hopeless and despondent. But yea, keep that model up cause that’s going to help solve prison overcrowding.
Adam, in the most difficult times of your life, don’t try to bear the pain of life on your own. Don’t try to bear the heavy load,
Jesus said: “come unto me, all ye that labor, and are heavy laden, and I will give you rest. Take my yoke upon you, for my yoke is easy, and my burden is light, and you shall find rest unto your souls.”
Pray this prayer:
“Heavenly Father, Holy be thy name, I come to you tonight with a shattered life and nowhere to turn. I come to you tonight without peace, without joy, without hope, and seemingly without a future. Father, please help me overcome this most difficult time in my life. Please give me your peace and your rest and deliver me from every sinful thing I have done in my life against your righteous ways. Help me to keep you righteous ways, give me a wonderful future, and I will forever praise your Holy name. Amen”
Thank you, Pamela. I actually had no idea of the scope of the problem until I started reading your columns. I’m glad you have such a social media presence so that people in general, but especially other doctors and also residency training program directors can learn from this.
I’ve mentioned my own issues with you before, but I just thought of something else: Between 1985-1990, there were a fair number of intern and residents committing suicide. The timing co-incided with the emergence of AIDS and the fact that there were no blood draw “teams;” the interns got the job and suffered from the pricks. It was a very scary time. At the hospital where I worked at that time, the head of Medicine requested from the head of Psychiatry that a group be run for trainees. I offered to do it as long as I received supervision in group therapy. One of the important parameters of the group was that it would be for interns only. This was because, as you know, sh** flows downhill and there would be plenty of payback for any interns who complained to residents. I did this group for two years, with two different groups of medical interns. I’m just mentioning this now to you because it could be built into a training schedule as protected time (residents had to cover for interns for that one hour) and it seemed to be a good forum for the group of interns to grow closer. In no way am I suggesting that this is all that’s needed; far from it. But the experience just popped into my head as I was reading your email this evening.
Excellent idea! We absolutely need more group coaching & healing opportunities as medical students, interns, residents, docs. Thank you for sharing this Susan. Much appreciated.
Please read the article linked above. What I don’t like about the tone of the article is the subdividing that the author uses in classifying the victim…”one of ours”….(meaning Anesthesiologists)….”our family”….(again meaning Anesthesiologists) This mindset needs to change. Anesthesiologists are part of the larger group called Doctors, who are part of a still larger group called Health care workers. You are genuine and I believe sincere in documenting suicide amongst doc’s. However I would wager that if expanded to include ALL health care workers, PA’s, Nurses, etc, etc…..that work in critical care environments, you will find a disproportionate number of suicide’s, divorces, drug abuse and depression. There are multiple factors that contribute to these problems. Physicians are one subset of a much larger group. You identify many of the causative factors in your writings, however there are many more, and to ignore them only serves to leave so many others suffering within the system without a lifeline. I know this is not intentional.
The oppressive nature of the system as it exists presently is a massive problem. Doc’s are most certainly abused by a heartless, oppressive, cold, dehumanizing culture. That culture permeates everything in health care. It is because the system is sick, that the participants within the system become ill also. I applaud your efforts to bring these problems to the public at large. I just want to make sure that we don’t lose sight of the larger picture. Again, I applaud and commend you for illuminating a problem that has existed for far too long. I hope that your example will encourage others to come forward.
I totally agree with you and I always welcome depressed & suicidal health care workers of all sorts to the retreats I offer. (massage therapists, RNs, veterinarians have all come in the past).
Also I have a separate list I keep with other health care professionals. For the purposes of the film the focus is on doctor suicides. Lessons learned can apply to all health professionals I’m sure. I do not want anyone excluded.
~ Pamela
Fantastic article and research Pamela. You are one of the first beacons of hope in my lifetime illuminating the truths of the diseased medical system which cost the life of my brilliant and beloved father, a pioneering surgeon and in turn influenced the suicide deaths of two of my siblings.
Medical culture and training reform is long overdue and an idea whose time has come.
Infinite thanks from myself, my family and so many others in this healing journey for us all.
Thank you Sarah for being willing to share the pain that your family has endured since 1967 with no answers—until now. May this documentary shed light on your beloved father and the tragic loss of your siblings. The grief is unbearable. Suicide is preventable. May your family heal and be part of the healing that the medical profession has needed for more than a century. Thank you for opening your wound for the world to see & feel . . .
I am very proud of Dr Wible for been a female doctor who addresses suicide in physicians the way it is, without fear. Thank you!!
We need more fearless female physicians.
keep up the good fight , Pamela
Thanks Tom, but it’s not a fight; it’s a labor of love. <3
Pamela, firstly you have done and are doing amazing work,I hope you start to get more support from the AMA and others.
I am really saddened to hear things are so bad in the US. Having trained in the UK in the late 90s conditions were finally improving and have continued to improve with much more acceptable hours. Working now in New Zealand I think there is a more accepted culture of trying to achieve a good work/life balance.
I really wish you well with your amazing work.
Thanks Melanie! Yes, I do feel support is coming now from our medical organizations. The awareness among physicians of the humna rights violations and the public outcry for change is right around the corner.
Hi Pamela and Melanie.
Great informative needed work you are doing Pamela .
I also trained as a New Zealand doctor and there used to be a better wwork/life culture but the pressure is really on the younger generation in their residency and training years.
We have never worked the insane hours like US docs and I dont know how anyone can survive that system.
I have now been working in Australia in remote rural hospitals where GP generalists get very well paid but have onerous hours and responsibilities.
Not surprisingly younger docs arent keen to work like that and there is always a shortage of remote area docs,nurses and allied health.
We are all facing a mental health crisis .
This is rising in the general population with so many anxious stressed people as patients pushing their stress and demands onto us and we are not supported by the beauracracy or our managers who keep demanding more for less.
I am now nearly 60 and although I have enjoyed some great times in general practice and met some amazing people I cant recommend it as a career anymore especially if you would like a family and good relationship.
I work in the Social Work/ Community area and there are a lot of similarities.
Very sad. Doctors are under tremendous pressure, professionally and personally.They need more help than anyone else in society.
They (especially med students & residents) seem to have no real legal protection. Need help desperately.
Pamela,
Your work is a great gift to medical professionals, their families, patients, and communities.
I went into medicine to help people, but dropped out of medical school in my first year because it medical school seemed inhumane. I had to see a psychiatrist to get out. “You must be crazy to give back a 4 year, full-tuition fellowship at U.C. San Francisco.” But I knew I’d be crazy to stay.
Too many doctors are in a no win situation, but as you have proven, it doesn’t have to be that way. That you for all you do.
Thanks Jed. I’ve been up for almost 3 days (more sleep deprive than a resident) cold calling families in obituaries about their loved ones so we can have them in the film.
teach them to eliminate what is killing them and not themselves
he who seeks to save his life will lose it (being submissive and pleasing others)
he who is willing to lose his life will save it (reclaim your true life and eliminate the untrue life imposed upon you)
ask yourself why you became a health professional and if the answer is not about caring for people you have a problem because people bring the problems to their doctors
how about nurse suicide rates?
they want to help everyone how does that affect them?
being unable to say no when asked to do things by friends and family they do not want to do is a big problem for nurses
health professionals don’t teach or live survivor personality behavior
go to my web site for many helpful articles and my books too. i felt the pain of not being able to cure everyone and sought the answers and helped to heal myself by living the sermon. a perfect world is not creation it is a magic trick with no meaning.
A third year psychiatry resident from our children’s hospital (Rainbow babies and Children’s Hospital) killed himself by overdose in 1995 and we were all forbidden from attending that resident’s funeral. Because our pediatric attending (who sucked) told us “This is an occupational hazard of this job. You need to come to work and do your job.” ~ Nora McNamara
A third year psychiatry resident from our children’s hospital (Rainbow babies and Children’s Hospital) killed himself by overdose in 1995 and we were all forbidden from attending that resident’s funeral. Because our pediatric attending (who sucked) told us “This is an occupational hazard of this job. You need to come to work and do your job.” ~ Nora McNamara
I was in medical and was going on for a PA from RN but after two years Quit because I couldn’t handle all the patients alone . They were sick and don’t understand the paperwork involved and red tape just to help their pain . I would be stuck with 30 all alone ! Well fast forward 15 yrs I’m starting to get sick so 4 months ago I’m dx with Lupus which is an entirely different story but what I’m trying to say is I’ve now been on both sides of medical . I see it crumbling . A Dr ,or anyone in medical should never ever be forced into risking their great talents for a corrupted bunch of money hungry imbisals ! I have actually calmed others down while in waiting on my Dr who was called to an emergency at hospital explaining why they are waiting hours . I gave one lady 50.00 gift card ( I didn’t need it) to calm her down because she was in waiting area 3 hrs & I seen the stress and she started cussing the office staff who truly are sometimes clueless and should be trained to explain things and show compassion because patients don’t understand what’s going on and the tons of aggravation a Dr. faces . I had that waiting area in complete calmness by simply explaining & listening to them. I was so sick that day but I knew somebody had to do something because the Drs and other nurses would be blamed and oh God nothing worse than hearing a patient cuss you out and degrade you for stuff out of your control ! I’ve seen Drs go off and stand alone as if they had nobody who cared . Where’s their hug or thank you ? It’s pitiful ! ( I give my dr sports stuff for his favorite team because it’s gave to me , I try small things to return the kindness my dr shows despite sometimes Drs who know my background take for granite I’m to know certain things and I’m left basically saying what blood work I’m needing lol I don’t know everything and it’s something learned everyday ! I can say this …The DEA needs put in their place and you guys shouldn’t have their rules . I say stand together & continue treating your patients your way & as far as opioids , I honestly think that’s a Dr and patient decision , not DEA or pharmacist . That’s adding to the stress DRs face ! There’s got to be a way ALL Drs can do what they love without criticism and dictators . I am in agriculture now and I love it but I loved medical as well . Don’t give up on something your called to do . Its a gift that very few can do! Your a family & maybe some of you can join in and get your own practices together and practice medicine as it was intended . We need you & not for just pain medicine ! We need hope there’s a better tomorrow & numerous other things ! I wish patients could understand what’s going on with you guys as well as them . I apologize for the long reply , I’m just trying to explain things as I see them and let each of you know your needed !so band together and take back what you were trained to do and make time for yourself & family ! We each know life is short!!!
Thank you Kim. We need the equivalent of a WalMart greeter and clinic/hospital peacebuilder at every medical institution. Addressing underlying system dysfunction first would help. Prevention is the mainstay of good medical care & service.
Excellent column, Pamela.
I take issue with the assertion that residents are ever “sent to psychiatrists for stimulant medications”. This would be unethical behavior on the part of whoever is doing the referring, besides which psychiatrists rarely if ever prescribe “stimulant medications”.
A resident might possibly be diagnosed with narcolepsy or ADHD, but this would not normally be treated by a psychiatrist, and at any rate, the treating psychiatrist would decide which medications to prescribe if indicated.
Some reports have noted that a large number of today’s students have long been on ADHD medications. Some even more disturbing reports are emerging that PHPs (even non physician PHP directors such as psychologists) in their zeal to promote strict abstinence programs for all clients regardless of diagnosis, have demanded that students and doctors come OFF their ADHD or narcolepsy or OSA medications so as not to interfere with drug testing for substances of abuse.
Stopping a legally prescribed medication for a potentially life threatening condition is medically indefensible, unethical and illegal, if it is done by a nonphysician.
Excellent column, Pamela.
I take issue with the assertion that residents are ever “sent to psychiatrists for stimulant medications”. This would be unethical behavior on the part of whoever is doing the referring, besides which psychiatrists rarely if ever prescribe “stimulant medications”.
A resident might possibly be diagnosed with narcolepsy or ADHD, but this would not normally be treated by a psychiatrist, and at any rate, the treating psychiatrist would decide which medications to prescribe if indicated.
Some reports have noted that a large number of today’s students have long been on ADHD medications. Some even more disturbing reports are emerging that PHPs (even non physician PHP directors such as psychologists) in their zeal to promote strict abstinence programs for all clients regardless of diagnosis, have demanded that students and doctors come OFF their ADHD or narcolepsy or OSA medications so as not to interfere with drug testing for substances of abuse.
Stopping a legally prescribed medication for a potentially life threatening condition is medically indefensible, unethical and illegal, if it is done by a nonphysician. And if it leads to morbidity or mortality, well, then we are potentially dealing with intentional infliction of emotional distress/suffering/illness or even murder.
The entire topic of prescription use/overuse/abuse among med students/residents needs further investigation. I’m horrified by what I’ve heard from those forced to receive psychiatric care for “inefficiencies” on the medical assembly line.
“I was told by the psychologist at my med school’s campus assistance program, that 75% of the class of 175 people were on antidepressants,” shares psychiatrist Dr. Jaya V. Nair. “He wasn’t joking. How broken is the system, that doctors have to be pushed into illness in order to be trained to do their job?”
“During my internship, I found out that at least 75% of my fellow residents were on SSRIs or other antidepressants, just ‘to get through it’ because it was so horrible.” states Dr. Joel Cooper, “Depression, or a constantly depressed state, is more or less the norm in medical school and throughout one’s residency.”
“When I left my residency, I was alarmed to find out that about 75% of my fellow residents had started antidepressants since their intern year,” says Dr. Jill Fadal.
More here on this epidemic: https://www.idealmedicalcare.org/blog/75-med-students-antidepressants-stimulants/
(of course another symptoms of meded gone awry)
As a second year resident I stood in a patient room on the top floor of our hospital and wished the window opened so I could jump.
I promptly realized the severity of these thoughts and sought help. Part of me worries about my “record” of MDD (and OCD) and what it means for my future as a physician.
The thankfully louder part of me is now very open about my mental illness, treatment and experiences. I want others to know that asking for help is ok. Having depression, anxiety, etc does not make you weak. I hope my openness is a catalyst for change in my medical community.
I very clearly remember one lecture as a medical student about to start my internship. The topic was “you will kill patients, and this is how you’ll do it”…
Dear Dr Wible, thank you for speaking up for doctors. Your article “What I’ve learned from 547 doctor suicides” summarises so much of what is wrong with the medical profession. I am a cardiology trainee, and the expectations of the system on myself and my colleagues is brutal. It has made all of us into the worst versions of ourselves, and I am ashamed to no longer be able to care as much as I used to. I hope that change towards our work culture will continue to happen, and wish you all the best.
Thank you so much for bringing this out in the open. I too recently spoke up about suicides occurring in corporate Australia – by the C-Suite of professionals. Again, in a room for 22 people, we have 6 directly affected by a suicide of someone, most a direct report!!!!!! I too became a quasi-suicide hotline.
Suicide is a public health crises – a GLOBAL public health crises. Thank you
Thank you for being a truthspeaker.
Lost a dear friend, and world-acclaimed physician to suicide years ago. He was brilliant, tender hearted and physically blessed as a competing triathlete. He was written about in the book: WALK ON WATER. I’ll never get over it.
Who was this doctor? Do you have an obituary? Are you in touch with family? We can honor him in film if we have family approval.
Dr. Jonathan Drummond-Webb ❤️🩹
really impressed that you have contributed so much on this topic, this hidden and stigmatised issue that needs full exploration. Well done.
Labor of love. Couldn’t keep watching so many doctors go down without doing something.
HOW PATIENTS CAN HELP DOCTORS NOT KILL THEMSELVES:
“Hi Dr. Wible, An acquaintance posted one of your articles about physician suicide online. I have multiple chronic illnesses (metabolic syndrome +) and so I see a few doctors. They are all residents, as I live near the University of Michigan. I am lucky as they are wonderful but I am also concerned about them after reading this. Although there is zero chance they would share something like this with me, of course, is there any way for patients to support your efforts to prevent physician suicide? I would be devastated if any of them killed themselves. When I was hospitalized with high blood pressure, I wrote all of them thank you notes, specifically noting their strengths in treating me. I’m sure they all found this somewhat weird, as the caring we receive from doctors is largely a one-way transaction mediated by money in our society. In any case, thank you very much for bringing light to this issue.”
My answer:
The thank you cards really help.
Even if docs don’t show it – they are touched.
Keep doing that. You can also ask:
1) How are YOU feeling?
2) Did you get any sleep last night?
How long have you been on shift?
3) If they seem like they are starving
hand them a power bar (keep little
snacks with you to share)
It’s simple things like this
that make all the difference.
~ Pamela
Great article! I have a dear friend who lost her physician husband to suicide. Hope his sheds light on things she has thought and felt for years.
Please do share his name or obituary.
Neil was 2nd. year student at University of Massachusetts Medical School. He was 6 ft 3 in tall, smart, great personality and was known as Demi God among his friends.
One day before thanksgiving in November 1998, we lost him at the age of 23 years.
Our younger daughter, Meera Grover, also graduated from University of Massachusetts Medical School in 2004. The school and his classmates have a bench in his memory at the school and a Neil Grover Memorial Scholarship awarded every year.
After Neil’s death, we started going to a Grief Sessions held in Springfield, MA under Mary Pat McMohan, who had lost her son at the age of 22 years. We became a family of our own. The interaction with other people helped us to become little stronger every day. With so many sad stories at the grief session,I wondered how I could make other parents and sibling aware of this illness.There were all kind of Walks except no formal Walk on Suicide prevention.
I told my idea to the grief session group. There was a dead silence on this idea. They were all worried that this idea would not work as there was so much Stigma attached to this cause. I did not give up and started pursuing for a location and got many rejections. I did not tell the group about the rejections. There was a myth that if we talked about suicide, it would happen.
Ultimately, Jewish Community Center in Springfield gave me the place at no cost. I would always be thankful to Michael Paysnick (The Director) for his sensitivity of the cause. He knew Neil. However, he expressed his concern that I would not be sad if not too many people joined me for this Walk. My answer was that even if 10 people walked, we would be bringing awareness, to the community.
In 2001,with full support from the grief session group, we had about 250 people at the first walk with no TV coverage We had a picture on the third page with a small write up on the third page of the news paper.
We had named the walk as” The End of Secrecy”
In 2004, American Foundation for Suicide Prevention made this as formal Community Walk named as ‘Out of the Darkness’. It is now in more than 365 cities.
Currently , I help the cause by anyone wants me to share the story. At the last Springfield Walk, we had approximately one thousand people.
Dr. Meera Grover is an Anesthesiologist at Brigham and Women Hospital in Boston.. We have three grandchildren who participate in the Walk. They always ask about Neil..
Neena grover
“Male anesthesiologists are at highest risk. Most die by overdose. Many are found dead in hospital call rooms”. Hits VERY close to home for me- the primary reason is the extreme pressure working in anesthesia. I’ve had a schoolmate commit suicide in the call room, have sent another to drug rehab. It is a job that take a high toll. At least for me, between working ICU and then anesthesia- a part of me died with each patient I lost until I was dead inside. Been out for 15 years and am still recovering from it…I suspect one never fully does recover. Between being ICU charge nurse and then anesthetist for 20 years the stress was too much and I had to quit to save both my sanity and life
Hi Diane.
My name is Angela and I’m a freelance journalist writing about suicide among male anaesthesiologists–I understand this is a sensitive issue but it’s also an important one. Would you be interested in being interviewed me about your experiences? They sound important.
My email is angela(dot)skujins(at)gmail(dot)com. I can provide anonymity upon request.
I know a woman who was a year ahead of me in an anesthesiology residency. I think of her often. I was starting to get to know her better and she was confiding in me some of the problems she was having. She had married an attorney who turned out to be very controlling and abusive. They divorced. She was physically drop dead gorgeous, which she felt got in the way of relationships since men could not see beyond her looks. I barely could, either at first. Even in scrubs, her physical beauty just radiated. But she was also so smart, funny, interesting-and very lonely. She started an IV on herself with the “usual” anesthesia cocktail and ended her life and suffering.
I had gotten to know her better when we talked as she “kept on eye” on me during my coma from taking 11 grams of barbiturates (and after a week, life support was being removed, papers signed for organ donation, etc)…. and then totally unexpected….very shortly before life support was to be turned off, I started to come out of the coma. In one conversation, she asked me about other methods I had thought about and I did mention the IV route, but did not think I could manage that. And then the following week, she died and we never had the lunch date that we had planned for that next week. Decades later, I think about her and ache for the pain she had. So she will be an unnamed, but remembered person in the film.
Hi anon.
My name is Angela and I’m a freelance journalist writing about suicide among male anaesthesiologists–I understand this is a sensitive issue but it’s also an important one. Would you be interested in being interviewed me about your experiences? They sound important.
My email is angela(dot)skujins(at)gmail(dot)com. I can provide anonymity upon request.
Regarding the suicides of the brothers Drs. Gary and Jeff Reiter.
Pamela
Thanks for sharing this information. I find it incredibly sad that two brothers with so much love and support for others, who went into the same profession, and attended the same residency program ended their own lives.
Joe Pace was another good friend from school I’ve lost touch with. I resonate with his feelings and taking time off. During our first summer as med students we were allowed to go off on vacation in the summer for two months (a luxury at the time). Another classmate and I went to Europe riding the trains and backpacking. We ended up on the far side of the island of Corfu in a campground. As we were setting up our tent I heard a voice from another campsite. It turned out to be Joe who was traveling on his own in Europe! One of the few moments-memories I cherish during my schooling along with my friendship with Jeff and Jill (all of us were from California living in the foreign land of Wisconsin).
I want to add that advocating for proper time off for students and interns, residents, fellows is critical. My residency program in Internal Medicine essentially made us draw straws for which month in our internship we would get vacation. I drew the short straw and had to take the first month of internship as vacation. I came back from “vacation” behind all of my intern classmates with no time off left in the year. As you can imagine I went through a mini crisis after Jeff’s death where I felt that the training and setting for my internship did not support or look like what I wanted to be as a physician. I was barely “allowed” to go to his funeral were it not for my resident. I had been on call the night before and up all night admitting and caring for patients. My resident let me leave in the AM to fly to LA for the funeral (I made only the burial not the service). It all remains a blur to me except for standing alone over his casket in the hole at the end and putting a decal from our favorite band in his grave. I had to return that afternoon and come back to work the next morning. Later that year I went to my program director and told him I want to take the next year off. I spent that year working in the local outpatient clinics and assessing whether I wanted to continue my training. Fortunately I realized that residency training was not representative or indicative of the profession and went back.
I also took the year “off” between college and medical school to explore myself and the world before the big commitment. It was a year which I still cherish and have friendships for life. I have shared these insights and advocated to our medical students, residents and others that it is okay to take time off for personal and professional development. It should not be seen as a “gap” in your resume as long as your soul, motivations and goals are nourished. Now some thirty years later I find a new chapter in my career as I pursue developing and supporting a lifestyle medicine approach to my practice and our clinic. The vital signs of nutrition, physical activity, social engagement, stress management, and sleep have taken the forefront for treatment and prevention. Physicians and all healthcare providers need to check their own vital signs frequently before they go silent.
Unfortunately suicide remains a pervasive issue for everyone. It has been in the top ten causes of mortality in the US for several years. I recently had a good friend from college (non-professional) kill himself. As I reached out to others it was amazing (and disheartening) how many of us have known someone (or many) who took their own lives. It is a dialogue and advocacy that must continue for all of us until the underlying causes in society and our environments are addressed in a positive and supportive way.
Thanks for your work and please feel free to share this information as you see fit.
With gratitude
Jordan
Unfortunately I think about it every day . . . tired of taking drugs just to be able to go to work every day. I tried to go through a physician health program but would have to drive 6 hours for an appointment. What’s the point? Menial tasks and wasting time on the computer until midnight every night are making me hate my job more and more. I take more time off just to take longer to complete tasks. No time to read or learn. I “own” my practice though make significantly less than most family physicians. Actually insurance companies and governmental regulations own me . . . so I still practice assembly line medicine. I am just tired and want to quit. My kids will graduate in May. My job will be done. . .
I’ll email you now. There are answers if you want help. You don’t have to end your life or live in a state of despair. Please. 541-345-2437. Leave a message anytime and I’ll call u back if I’m with a patient.
Worst night of my career was admitting a colleague with a tricyclic overdose. Fortunately for her (and for me) we had access to a superb critical care facility and she recovered. She left medicine the day after she was discharged.
I have done emergency medicine and served in a combat zone – but this still haunts me most.
Oh that is intense. Did you have any debriefing? I can hook you up if you need to talk to someone. Don’t bury the pain.
Dr Wible
Thanks for all you are doing to improve things for health care professionals.
I had severe depression during my first year of family practice residency and my marriage counselor was able to get me through it with CBT.
6 years into private solo practice I heard a message of hope from a physician giving a CME presentation on alcoholism, who had seen his wife achieve the miracle of recovery and decided to focus on my own sobriety.
I stopped trying to fix my wife and developed a sober network of support and now, 28 years later, have an amazingly rewarding job as medical director for a growing addiction treatment company that has 34 facilities in 5 states.
I have facilitated group therapy for professionals early in recovery from addiction and observed many urine drug tests for the Professional Health Program. Some of these people are alive today only because of the case management of this program but I have also seen the onerous punitive medical board actions for those who did not do well in treatment.
I cannot blame my substance use disorder on the medical system as it clearly predated my medical training.
I am grateful that my illness has given me a wonderful final chapter in my medical career and recommend that those interested in helping, do the course work to join the substance use disorder treatment work force. The leading cause of death for people active in addiction is suicide.
Dear happy, joyous, free ~ so thankful you made it—and now you have the blessing and honor of being able to help others to recovery. Thank you for your work in the world.
I would simply like to add to your excellent work. I would look forward to potentially correspond with you pertaining to my wealth of experiences here in Sydney, Australia. This dilemma had recently reached crisis point in early 2017 with our junior doctors- but of course, the my state governments’ department of health response was predictably inadequate. Currently I’m not practicing,and I have now made it my sole career mission to properly address and formally approach my local and commonwealth government. I’m very proud to announce I have gone a step further, and I believe I have solely come up with a workable plan and I will be going national with it shortly. Hopefully if successful, it can be implemented worldwide.
Excellent please let me know how I might help.
Sorry its been some days, but firstly I’d like to instil an appropriate messages of hope to all of our colleagues worldwide who read your wonderful website. There is no doubt what we attempt to address here requires complex considerations to a multitude of what are sometimes diffuse but also quite individualised factors that seemingly evolve constantly over time.
The good news that I want to surface soon is that the pathway to get back and maintain our own good mental-being seems to be more linearly defined and whilst proactive, should certainly not need be over- reliant on specific well designed qualitative outcome studies that will take many years to complete and scrutinise.
Perhaps if I could discuss one important reminder today is the regular practice of what is now coined self-compassion. General surveys will repeatedly reveal we are the most highly valued of all the professionals in our communities. But my simple reminder is this we too are members of our society, and if we are truly valued, then its is time that we utilise this status but along with it ask this question; Why does its really need to be a big deal if an occasion of time comes along, ranging from where we either need to slow down in our work output to benefitting from receipt of some form of a helping hand from another health professional ?. Furthermore, what is it that obstructs us having permission to take time away from the daily hard-grind and role responsibilities to interrupt a potential spiral downwards? The first step I believe is the obvious above mentioned, and that is, we can all finally admit to ourselves that yes, we too are human (and so yes, we therefore cannot expect ourselves to function as “superhuman 100 % of the time”).
So it would seem to be about how we can transfer this more realistic expectation of what we are about and know how to transfer this so that our employers and patients(both of whom, can be unrealistically idealising of what is possible to deliver)can be even kinder and more accommodating than we can usually be to ourselves.
What I want to address is how practical health promotion can occur in our working lives- just hope that my government when they resume in our capital in a few weeks time still considers it an important enough issue to be urgently addressed still . Will keep you and all others advised of my progress.
I have just had a frustrating 6 months of waiting for the Gov’t to acknowledge that I finally even exist!
Seems like the Australian Gov’t thinks they have all of our problems solved; Yes, after contacting many times since,it’s taken me 6 months for our Health Ministers’ office to reply to me, and to then just be told for me to monitor a research website on my own accord, as apparently there is no funding.
Seems they are content on just watching the front-line Drs and nurses in our public hospital system continue to fall, whilst researchers continue to crunch their numbers and present their statistical analyses to the Minister sometime next decade for what will always remain qualitative and humanistic.
It is now apparent that this is a true a David Vs Goliath battle that I have embarked upon. But instead of beating my head up against the very thick brick wall that they have erected in front of me, I’ve determined I will look at entirely different approaches to deliver my completed work.
I am a firm believer in the benefits for all derived from what everybody has to agree can only be constructive creation- but if that doesn’t work, do I actually play that game of wait and see,suspend what I know what I have already achieved will work, and furthermore, can be the only meaningful outcome?. So, I shall do once more what we are quietly trained to do best;swallow my pride once more, forge forward and consider all other options. Any constructive practical suggestions from you or others reading this would be appreciated at this stage………….
Have a clear goal, reverse engineer the steps to get there, and don’t give up. Asking your oppressors for help will slow you down.
Hello Pam and thank you so much for your work. I am a Patient Educator/Standard Patient.
Every chance I get with our students I mention your name and try to find out if the student is ok. I educate around the stresses, and politely let them know that they are not alone. I do not care if I am overstepping boundaries: this issue is too imp. Today I gave your link to a Brigham and Women’s Harvard doctor who is one of the creators of Peer Support. I asked her if she thought we could bring this technique into medical schools. I am not an admin. but I do find the idea enticing. Again you are saving lives. The bio-medical culture MUST change.
Thank you so much Mary! We must do whatever we can to save each other.
WHO KNEW???? Thanks for the education and bringing this to light! What can people do to help?
To help:
Step 1) Raise public awareness (and decrease professional denial). Share articles & Do No Harm film. Links below.
Do No Harm film (view trailer here)
Physician Suicide 101: Secrets, Lies & Solutions
Free audiobook on doctor suicide prevention here: https://www.idealmedicalcare.org/books/
Please share widely. People have NO clue.
~ Pamela
I understand the pressures of the medical field. I cannot believe that the “fix” still has residents working 28 hour shifts! I pushed my daughter to pursue a different career. She found something else that she is passionate about. Unfortunately, two of her best friends are off to med school in the fall and this article makes me even more worried for them.
Dear Pamela,
That was the most honest and soul touching article I have read. It made me cry……
I currently have 3 physicians and one Nurse Practitioner in my practice that I treat under fake names and I don’t charge them…..they use Good Rx to get meds or just come to talk.
My office has gotten the reputation as “the Underground Railroad for medical people” which is wonderful but so sad and ironic at the same time. I have 1 person from Corvallis, 2 from Salem and one from Portland.
All know each other and I am the “go to….word of mouth psychiatric practice”……
Sadly one nursing student ended his life last year by an aspirin overdose and I was really blessed to have my favorite psychiatrist best friend help me process that suicide…..even I know to have support for myself in place…..it is critical to my own mental health….
Thank you for everything you do……… I know your work is valuable, needed desperately and so appreciated!!!!!
Bless you for your work. I am in constant wonder and concern about the expectations for physicians by their profession and from their patients. I never get adequate care from MD’s or OD’s in 15 minutes. So, I am very pro-active in maintaining my health and seeking care from alternative modalities and practitioners who for the most part still have time to listen to their patients, think about the best scenario and be present in the moment of caring as a professional. How can we expect other mere mortals to act like automatons in providing their patients care under the accountants dictums and not be affected by all the vagaries of life and death experienced in the healing arts? Again, bless you for your work and I hope the AMA is listening now.
“Med students and doctors often suffer in silence and isolation and often their deaths go unrecognized as but an “occupational hazard”. There are systemic failures in our educational and training programs and societal and professional stigmata that influence our ability to speak honestly and openly when suicide occurs amongst our colleagues and peers. My first experience dates back to the late 1970’s when early one morning I dropped into the local emerg department on my way to the doctors lounge. I was asked to wait as a “code” was in transit momentarily. The patient arrived and was moved directly into the crash room. The EMS attendants continued CPR while the nurses and emergency doc began their drill. And then, the recognition. The patient was a family doctor, well-known and respected in the community and by his peers. He was a sensitive and caring man, a published poet and active member of the family Medicine department. Cardiac event was the likely precipitating cause of his arrest, that is until I noted the needle stick wound in his left anterior chest. My colleague and friend had apparently injected potassium chloride directly into his heart. His death was precipitous. In the aftermath, there was silence, in the E.R. and the doctors’ lounge and department. Little was spoken of this tragedy in the weeks and months that followed. Nothing was done to prevent this from happening in the future.” ~ Howard Goldstein, MD
Doctor, would it be possible to talk to you about a doctor-friend of mine? He has really been “slipping”, and I feel as if he is cracking up under some kind of pressure. His memory is failing him and he is acting out. He has been behaving in a passive-aggressive manner as well. Thank you.
Yes. I just emailed you.
I just read your article and I am stunned. I did not know my experience was so common. I graduated from medical school in 2010. Since starting medical school I have known one neurosurgery resident die in a car crash due to fatigue, one of my former classmates died from an overdose of fentanyl, a resident at a hospital I rotated at died by suicide by leaping off the parking structure, and, just a few weeks ago, a resident at the hospital where my wife works committed suicide at work via GSW. Reading your article was like cold water in my face, particularly the following part. “If they “violate” work hours (by caring for patients), they can be forced to lie on their time cards or be written up as “inefficient” and sent to a psychiatrist for stimulant medications.” I was a surgical resident who struggled with lack of sleep in a program which eventually was put on probation due to duty hour violations, though we were bullied into lying about our hours. Any violations were our fault, not the programs. I was picked on by a more advanced resident, and the program director sent me to Employee Assistance Program because he thought I was the source of the problems. They sent me to a psychologist, who diagnosed me with ADD. He sent me to a pyschiatrist, who added Bupropion and Methylphenidate to my Escitalopram. I ended up not having my contract renewed in the end, and I have been struggling with feelings of inadequacy, failure, and low self-confidence since then. Just this week I started a peds program and I pray to God that the attitudes in this program are different than they were in my surgical program. I had no idea until I read your article that my experience could be similar to someone else’s. I have been so ashamed and lost about what to do about what happened to me during that residency. Thank you for writing this article. I still don’t know if there was a better way for me to have dealt with my situation (for instance, another resident took the program to court and perhaps I should have done the same) but it’s good to know that I am not alone. If you have any advice for me, I would love to hear it. Thank you so much for your work and bravery. ~ Joe
I remember reading about a doctor in Dix Hills, Long Island, NY that tried to kill himself by running his car in his garage. He survived, but the fumes went up into the house and killed his wife and 2 little girls while they slept. He ruined his life and went to jail. It is sad. People who take on the challenge of many years of school to serve their fellow man should be treated better. Thank you for your recent article in the WaPo. I look forward to that documentary.
Does anyone think that AMA is the problem and has been for decades, Dont you know the history of AMA And FDA? Do you know about History of Dr Koch Or Hoxey. learn about the way AMA treated them regardless of what they did or did not do. It seems the same practice was unlisted long ago. It makes sense that it is routine and well managed. It is learning about history, I see the questions i have make sense, It would be hard to do if i did not live or see it in the many post and issues social media has allowed. This is one thing they had to their advantage power and control. what a sick and unique way to profit, Both on healing and healer.
How can any of us maintain even a modicum of mental health when every day we are FORCED to deal with health insurances companies under an assortment of names, Health Plans , HMOs, IPA’s and many more who lie,cheat and steal to make as much money as they can by denying as much care as they can?
How can we prevent disease when fanatical, ignorant, rude people continue to spout lies about life-saving vaccines ?
How can anyone expect us to make life and death decisions day in and day out, to listen to patients for free at 3 in the morning, to try and practice the best medicine we can, while drug companies decide over night to raise prices thousands of percents , and attorneys who charge by the minute, sit ready to destroy us while state medical boards are ready to take away our license for any signs of stress exacerbating mental illness to the point of suicide ?
The question isn’t why there are so many physician suicides? The question is why there are not tens or hundreds or thousands of times more of them ?
“The question is why there are not tens or hundreds or thousands of times more of them?”
I believe these 757 are the tip of the iceberg. Pandoras box has now been cracked open and there are 10s of thousands of body bags full of suicided doctors. I’m also surprised there are not more. Speaks to our inherent resilience that so many of us are still breathing despite the chronic human rights violations.
I believe you are SPOT ON..It is the tip of the iceberg. Pandora’s box is cracked opening and I hear the creaking of it opening more and more….
I have a short poem, not really good poetry, but it does express more of my thoughts.
It is down below.
The pain of healing is hard to bear
Drug companies getting 1000s of times their share
IPA’s, HMOs, and Health Plans too
They steal way, way more than their due
So much work and so few thanks
While all the money flows to “their” banks
Little sleep and lots of worry
Being told, go faster, you must hurry
The plumber make way more per hour
While the doctor holds so little power
Would I do this job again?
No, it’s really just a dead end.
Thank you Charles. Spot on. I keep hearing the song: Don Henley The End of Innocence. This song came on the radio today and I couldn’t stop crying for my colleagues lost to suicide. Our innocence and idealism stolen. As I wrote in the opening paragraph of my book Physician Suicide Letters: “Despite it all, I remain an optimist. Medical school knocked me to my knees. I haven’t been the same since. Even though I still have a sparkle in my eyes and joy in my heart, a piece of me is missing. I can never get it back. I’ve tried. My innocence is gone.”
Just lay your head back on the ground
And let your hair fall all around me
Offer up your best defense
But this is the end
This is the end of the innocence
And all I could think about with that line was Dr. Deelshad Joomun stepping off the building at Mount Sinai to her death from 33 stories. A beautiful doctor in a white coat on the ground. Read my eulogy to Dr. Joomun.
Thank you so much for this article. I recently took the MCAT and am preparing my application to med school. But, as someone who has struggled with mental illness for years, this is a very scary reality. After reading this post and others like it, I question whether medicine is worth the mental anguish and it forces me to seriously reconsider trying to enter the field.
Email me. I’m happy to talk to you Madison. Please share your vision for your future. What field do you wish to pursue in medicine? Contact me here: https://www.idealmedicalcare.org/blog/contact/
Anything is possible. Contact me & I’ll fill you in on next steps: https://www.idealmedicalcare.org/blog/contact/
Wow! I never knew. I thought it was just psychiatrists who suicide. Now I have even more respect for doctors who care for me.
keep up the good work. I have a free ebook on physician stress. Anyone can email me for a copy.
I am wondering why do we need all these medical boards, residencies etc ?
Why can’t we work after we graduated medical institute ????
Before 90th it was on a free will if you want to advance your career if you wish to be a surgeon etc but you still CAN work after your graduation of University as a GP
Why any doctor must deal with financial matters????
Our business is to treat and save AND NOT TO COUNT BILLS!!!
Medical care MUST be paid by government for ANY person in country and it MUST be free !!
We are not Gods- we are human beings and can’t do everything. Some illnesses can’t be treated – NO ONE CAN PREDICT WHEN ,HOW AND FROM WHAT HE WILL BE GOT SICK- SO WHY DOCTORS MUST BE BLAMED AND SUED FOR HELP THEY TRIED TO PROVIDE????
ALL MEDICAL PROFESSIONALS MUST BE LEFT IN PEACE . THEY MUST WORK IN AMBIENT, FRIENDLY ATMOSPHERE WITH ALL RIGHTS
ALL THESE SPECULATIONS ABOUT MEDICAL BOARDS AND CONTINUES MEDICAL EDUCTIONS MUST BE STOPPED !
DOCTOR IS FREE PROFESSIONAL AND CAN PROVIDE HELP TO WHOEVER AND WHENEVER IF HE IS ABLE TO DO IT. IF NOT -THEN NO ONE DARES TO JUDGE HIM !
I hope my comment will be read by smart and intelligent politician or person who can start to change this system before all doctors will become desparate about their lives!
Dear Dr. Wible,
Two residents have killed themselves within a single month at NYU Langone. One of them hanged herself in my fiance’s building. The building’s windows were jammed to not open more than a couple of inches after another resident jumped to her death two years ago. I guess they thought this, and offering student counseling services would stop residents from killing themselves. A part of me wants to apologize for that last sentence, and ward off my cynicism, but I won’t; because, as you said, we need to shine a light on medicine’s dirty little secret before it’s too late. There are posters offering counseling services, and “heart-felt emails” being sent to the students, but here’s one thing no one in power to help is mentioning: The PI, the supervisors, and their bullying. (edited remaining portion to protect the person who submitted this post).
I’ve heard so many stories like this. OMG. I’ll email you. We must talk.
I am an anesthesia tech, I have been for 16 years. I am horrified at how little support staff, or uneducated support staff that anesthesiologists are expected to accept. The public has no idea about physician stress,inhuman working hours and lack of support from hospital administrators. It’s so wrong. I applaud your voice in this important work. Thank you!
Janet
Interesting that you should mention working conditions for anesthesiologists as I just published this podcast a few minutes ago: Why are so many male anesthesiologists dying by suicide?
Hi Pamela,
I just listened to your podcast. This is such important work, in the last four years one of our team members has attempted suicide and one has succumbed to addiction, both were men. All the factors mentioned in your webcast were present, it’s heartbreaking. The OR is getting worse with pressure to save minutes and do it with less staff. Another factor, is the unintended consequence of the advance of technology coupled with patient acuity. It’s a bad deal, really sick people, less time, and less support. I think the nature of the physician is to fix, then quietly go and fix again,that’s getting harder and harder. Thank you Pamela, wonderful work. Janet
Please share with the OR team—especially male anesthesiologists <3
I haven’t contemplated suicide. I have been an ER Dr for the last 20 years and recently was written up by Nurses for “patient abandonment”. A review found my care impeccable and the Nursing staff complaint to be not based on truth. Great. But the agony I have suffered in the last 2 months was excruciating. We live in a sick culture of blame. yet we work together day by day. I cannot yet explain their complaint. If I were a different person i would have considered this a “suicidal moment”. Why do we keep asking for absolute perfection from each other? yet daily we indulge patients, the worried well and the nursing staff, in their unrealistic expectations of our care?
Hello. I am a Paramedic. I read a story on NPR about doctor sucicides and it struck home with me. I have been struggling with suicidal feelings as a provider as well, and I couldn’t figure out why. What nobody is talking g about is how horrible the for-profit insurance system is and how horrible patients are. We see the same patients over and over and over. We see “failure to adult” over and over. We see people who think they are the most important thing, angry they got triaged for someone who is actually dying. We give patients everything. My compassion, my life is on hold for you. Yet it’s never enough. Patients can see a doctor and be prescribed the right medication but they don’t take it. They complain and whine that nobody is helping them. It’s a maddening, hopeless game out here some days. How do you help people who won’t help themselves? How do you help people people who make up illnesses for attention? How do you get alcoholics and addicts to stop using if they don’t want to? It’s SO frustrating to want to help people but they don’t truly want help. The depths of despair, uselessness, futility, and hopelessness can be consuming.
Part of a larger cultural catastrophe due to lack of mental health care in part. Many people are just playing out their unprocessed emotional turmoil on their own bodies and everyone around them. Victim-mindset + entitlement + lack of insight into the origin of their suffering. Complex for sure. Try not to frustrate yourself with the savior complex. You can only do your best and certainly take care of yourself first!
Hello, I am not in medicine but I definitely understand the topic. I live with CRPS/RSD (I was told the suicide disease). After being diagnosed and finding a support group, 5 people committed suicide. It broke my heart all because I know all too well of feeling as if no one cares or no one understands/listens. I love what you are doing to bring awareness that medical personnel may be dealing with issues that they may hide in fear of losing their license. Seeing traumata patients in the ER can affect them over time. They are not robots, they are human and have feelings and emotions. I would love to offer something that I created for the pain community to remind them/encourage them if they feel suicidal.
Fighter’s Creed
I, __________, will not give in to the pain. I will continue my fight for my life, family, friends, and others who may suffer from this disease. I know I am not alone and that I can still have a life. I control and own my body. My pain cannot define me but I can define the pain by which I learn to control. I will take small steps for I know the journey is long and hard. When I feel as though I cannot continue I will reach out to my support system and ask for help. I will speak and think positive of myself because I know I am worth it. I may struggle along the way but I will keep my faith. I will pray that my steps are steady for I know not of the ground I walk on. I will help others as we are all part of the human body. I will call 911 when I feel the need to end my life. I cannot bring pain to others yet help bring relief as best as I can. This is my creed as a fighter!!!!!
I know that it says “disease” but the message overall is to seek help. Life is precious and so are everyone in the world.
A.M. Styles
Thank you! Love this!!
Havent slept even 10 hours for the past week
Hi Dr. Wible,
I wanted to personally write you a message to say thank you for the work that you do. I used to work as a nurse practitioner. I worked 3 different positions before calling it quits with my career. I worked in very busy offices with impossible expectations. I was often left to run the clinic by the surgeon I worked with, and left with his work load as well when he would run several hours late (translation: two patients booked to see every 10 MINUTES!). I had a great six figure salary, attended my first continuing education at Harvard medical, and was highly respected……and I had never been so miserable in my entire life. With the high level of stress, impossible expectations set by patients, and impossible expectations set by the different offices I worked at I had become a terribly unhappy person. I was highly irritable, my hair was falling out, and it was starting to affect the personal relationships in my life. One day on my way to work at a stoplight, I thought to myself to just start running all the red lights because if I got into an accident and die at least I wouldn’t have to continue this life every day. Rather than doing that, I got the courage to leave the profession altogether. Today I am working as a state park ranger (having an undergrad in Biology helps!). It was obviously a massive pay cut and most everyone in my life thought I was crazy. However, I actually am happy again. I sleep well. My hairdresser commented that my hair has stopped falling out. My husband routinely comments on how cheerful I’ve become again. Simply put, I feel like myself again (plus 10 years younger!). The columns that you have written really helped give me the courage to make this move because I felt like there was no one who understood what I was going through (everyone I knew thought I “had it made” and how dare I complain about it). I actually like life again. Thank you so much for what you do!
Does data analysis exist correlating physician suicides by State, Training Program and Medical Board Intervention? How about by corporate medical company? Is such data different in single payer countries versus profit based insurance systems?
Your registry is critical to humanity. I lost mine navigating the complex (and often profit or politically motivated) reality of professional demands. Looking back my own tipping point occurred when the culture of medical delivery morphed from care sharing into liability shifting. I practiced hospital based medicine in
both academic and private settings.
I averaged over 80 hrs/week, many times over 100 hrs/week. As years passed by a divide emerged within the common, shared mission towards providing service to all patients. New arrivals of physician executives with little bedside experience began creating policy and procedures. Those of us functioning almost exclusively as clinicians often became labeled as disruptive. For example, discharging patients in the evening hours became at worst prohibited and at best a cause for the hospital employees to record complaints. It didn’t matter that the evening discharge best suited the patient while contributing to hospital earnings. (Those beds, when filled same day permitted double room Billings.)
What mattered most was the hospital systems need to over staff during the day and understaff during the evenings.
This produced a daily double bind for me, and catastrophically impacting my professional life, physical health, parenting and my marriage.
I am not alone. I now know of many physicians who experienced the devastation of anonymous medical board complaints (“Why else would he discaharge a patient at night unless he was on drugs?”, or “He takes a midday nap, who else does this that isn’t using drugs?”.)
Medical Boards publically release “accused” physicians, yet bury in their subsequent proceedings the vindications.
These vindications cost tems of thousands of dollars and many times much more to the physician. Yet at the end of it all no remedy for expensive and misplaced efforts exists for the reported physician.
It’s as if if there is smoke there is fire. All subsequent professional administrative tasks must repeatedly disclose being investigated, and not what the findings delivered. The impact is cumulative and not exhonorati g over a lifetime.
I find it totally understandable, and at times when advisable, to avoid at all costs interacting with one’s State Medical Board. Yet, some avenue must exist for physicians to reveal and offer insight into what they are experiencing, especially as it relates to patient care.
Thank you for your work. I am most happy to support your efforts
Themes are certainly emerging. “Punitive help” is most unhelpful when suffering with occupationally-induced distress.
I’ve had some thoughts about the duty restrictions and started writing a response to your Friday post re the duty hour petition… and lol yikes my response got long, and included my personal experience tangents that I do have a point in stating and tying back to my opinions on changing duty hours back… but anyways so below I cut and pasted the response I was typing up. Thought you should read it first
I can only speak from my personal experience in training, which crossed over the years when duty hours changes were being made. My rotation years as a medical student were from 2010-2012 and we had no restrictions; an example, my very first rotation as a Med student was OB where I did 32 hour shifts.
New Duty hour restrictions for residents began in 2012, my PGY1 year. I was a surgery resident, and the program I was at had done a really good job at creating appropriate shifts for residents, and I never had to do a single note or chart at home (that’s when dictating was allowed and they were strict on timeliness of dictation prior to shift ending. This was great; it taught us how to learn to become efficient and also to never be behind in charts).
I transferred into a Family Medicine program my PGY2 (2013-2014) year, same restrictions in place… and the experience in regards to shifts and abuse of the junior residents was shocking. And this was family medicine, not surgery. Not many cared if a resident lingered around for hours to complete notes. Attendings/ seniors that ‘maybe cared’ would say ‘if you have to complete charts after your shift you can’t be visible to other faculty and staff because of duty hour restriction’.
Every night during my time in that program I had charting to do in the evenings up until I finally made it to bed.
As for residents reporting number of hours spent working, lol yeah the residency tells you how to answer that to. They basically state the message that if residents have frustrations with hours or anything with the program, to not take your emotions out on these national surveys because that only hurts the program in the long run, such as a program ending up on probation. And who wants to graduate from a program in probation? Or piss off the program director and attendings whom hold all the power to the fate of your future career in their hands?
And this I know for a fact is true, because during my time in the FM program, I eventually sought out legal advice and representation because of the extreme abuse going on at my program.
Did you know that residents do not have any legal rights such as an employee does? In Law, a resident is seen or classified such as a student would be, not that that means anything, just how my lawyer explained it to me.
Did you also know that there are no regulations, or strictly enforced ones atleast, requiring documentation of a residents entire in-training experience?
Your faculty can make up ANYTHING about a residents training, good or bad. This absolutely happened at my program. It was horrible.
Also, yes residency programs across the nation are bringing in new mental health resources for residents in a program, BUT no one at a university, such as the GME, regulates if a
Program Director is actually utilizing and referring their residents to these new mental health resources. And I can also speak from my personal experience that that was an absolute fact going on at my program. Absolutely horrifying.
But on a more reassuring note, once the University GME Director found out about this happening within the FM program, an emergent meeting with all staff and faculty was made to take place 24 hours after the fact, canceling clinics etc because attendance was strictly required, and I remember all the faculty and staff gone, in a four hour lecture given by the GME Director, reviewing all the policy and procedure regarding mental health concerns for any resident, medical, and faculty and staff of a program.
Also at this time, the PD was asked/required to resign at the end of that year and the GME Director made it mandatory for the program to appoint a new program director within 30 days during the time this all happened.
Over the years I’ve been wanting to write out the things that happened to me during my experience in residency.
And I have thoughts on what really needs to happen in this country (and world) to effectively intervene and begin to hault this epidemic of losing our doctors.
Dear Dr. Wible, your video really touched me. I was doing some research on physician suicide when I found it. The reason? I have a great-grandson who will be graduating from high school in May. His aspiration is to become a psychiatrist because they don’t do much physical medicine, but make a lot of money and just hand out pills. I don’t know if he really feels this way or this is his happy-go-lucky way of covering up why he really wants to do it, but I plan on writing him a sincere letter to rethink his plans, if this is the real reason (which I don’t think it is). I recently retired from 50 years as an RN and am grossly disappointed in the medical profession – both in how they are taught to treat patients medically, and in the horrible stresses they are under. I know that most get into the profession because they really want to help people, but medical school usually totally squashes that in them pretty quickly. They are unhappy with the schooling, the system, and almost never being able to really help patients – only to medicate them and then watch them slowly die from from the side effects of the medicine. I watched my own husband be killed because of a stupid treatment ordered for him in the ER. I suspect it was an intern who did it, but just let it go. Nothing could bring him back. My wish for my great-grandson is that if he wants to get in to medicine that he would pursue a path that really helps people. It’s so much more satisfying to work daily knowing you are helping people to stay healthy. To experience their love, gratification, and gratefulness over having them taking care of them. After having surgery for cancer myself last year, I began researching natural medicine, foods, herbs, etc and have found a whole new world out there that I never knew existed. This is the direction that I would like to encourage him to take, because it is so, so needed today. Unfortunately insurances and Medicare will not pay for visits to a doctor that follows this path, so I’m not sure exactly how to make this sound appealing to him, or to even taking advice just from ole Gramma! I am interested in knowing what kind of clinics you are setting up that I may make something like that sound more appealing to him. Any information about your clinics that you could send me I’d greatly appreciate. Thank you for the path YOU have taken!
Maureen, so important to go into the profession for the right reasons and with informed consent of what you are signing up for. Have him listen to this free audiobook. I love my profession and when practiced with the right approach, medicine can be a very fulfilling and meaningful career. Do not pursue medicine for the money. There are far easier ways to earn a livelihood!
Excellent piece of news about cracks in the US medical health care system due to arrogance of Medical Boards nationwide surfing with their hypocritical ‘old boys’ club mentality. They know well through their scriptures that ““To error is Human and to forgiven is Divine” but they fail to acknowledge it.
Is there any literature on the relationship between physician suicide and/or depression and childhood abuse, trauma, “adverse childhood events”? I have been looking for it, and have not found anything. But it makes me wonder. I think most of us have been through the bullying, the losing a patient, all those terrible events which can happen during the course of a medical career. But not everyone drinks, or does drugs, or commits suicide. Any thoughts on what promotes resilience in the medical profession? And thank you for the work you are doing to bring the issue into the light.
Hi Martha, I would bet many of us have adverse childhood events and I have noticed some that choose emergency medicine seem to have more ACEs. Not sure if this has been officially studied. More data needed on doc suicide all around. Thanks for your curiosity.
I think that the thing that prevents medical students and residents from speaking out is the overwhelming fear of pissing the wrong people off and effectively ending one’s hopes of ever becoming a doctor. It’s a huge, huge fear in my opinion. And, in my judgement, it is just this atmosphere (where there is no recourse against recurring and possibly much greater petty, malignant, and toxic behavior) that underpins the sense of helplessness that leads to these suicides. But, do you know what is almost as bad? When, once you are a practicing physician, you can be made to feel just as helpless. When I worked as an anesthesiologist at a community hospital, I was told point blank by the anesthesia department head that anesthesiologists were the “whores” of the OR implying that I would not be treated any better than a whore. The surprising this is, she was exactly right. What proceeded after that discussion was nothing less than a nightmare for me personally and later, for her as well.
Regarding sexual harassment in residency (published with approval and de-identified email from a surgery resident):
Hi Dr. Wible
I was sexually harassed by an attending. The program backed the attending really hard and informally found both parties at fault for the “misunderstanding.” I was never interested in this creep and never led him on. He went on to harass other women in the program who chose not to report after seeing me be penalized for reporting. It ruined my relationship with my program director, who seems to think I led the guy on and lied about it.
I was groped repeatedly while operating this year. I told the man to stop touching me and he got thrown out of the OR. Afterwards I begged everyone not to tell my program as this would certainly be seen as my “second strike.” I suffered clear PTSD symptoms afterwards, nightmares, extreme anxiety crippling my ability to work; I tried to go to counseling but couldn’t leave work for it. I was sneaking into bathrooms to cry between cases. Eventually my performance took a hit, I wasn’t sleeping, I used a sharp tone with a nurse and got written up, and the man said he didnt mean to keep touching my breasts so everyone let it go and accused me of “making a big deal of nothing.”
The program offered me the choice of academic probation (a permanent sanction on my record) or resigning, and strongly encouraged me to resign. They won’t let me transfer due to my bad standing in the program.
I am so miserable that I am tempted to leave medicine – I don’t see any way of having a career survive this – but I haven’t always been so miserable, I haven’t always wanted to leave medicine, and deciding to leave while I acutely have PTSD and anxiety seems short sighted.
I requested to take medical leave and they initially said they would look into it, but because our program is so short-staffed and they need me for coverage, they’re not approving the leave.
My contract allows 30 days for victims of sexual assault, but they’re saying the man “accidentally bumped into me” so I believe they’re setting themselves up to say I’ll need a sexual assault court conviction not “just an accusation.” I doubt we’ll get a conviction in court; the man says he didn’t do it and that’s pretty much a he-said she-said
Please help.
Dear Dr. Wible:
I was a student respiratory therapist, and worked with a moonlighting Medical Resident, who covered our hospital on what few days he had off.
He was the best of the clan, who covered our 220 bed community hospital. I became a therapist near about the time he completed his fellowship, and he encouraged me to follow him to another out-of-state University Medical Center, where he was joining the staff.
I pondered the thought but declined his most generous offer and implied compliment. Years past, and I went onto become a Physiologist and a clinical researcher. Low and behold, I was visiting the town of my old highly esteemed friend and looked forward to a reunion. When I called the department of the University Medical Center, and asked for him by name, the receptionist receiving the call was stunned and indicated that I needed to speak to the department chair, as the doctor I referenced had died. In a state of disbelief, I queried her, as he was just a few years older than I, she indicated it was suicide.
Thoughts of Arlington’s poem: Richard Corey raced through my mind, how in the world could this have happened to someone bound for preeminence? In later years, I would visit the hospital and the staff remained hushed at the mere mention of his name. Finally, one day I encountered an older near retirement physician, who knew the circumstances quite well and understood why I was so perplexed, as he was brilliant, dedicated but he judged himself without mercy and was prone to depression. Such a loss to many patients and to the profession of medicine. His name should have appeared on the cover of textbooks but now a simple google search does not render his name.
I am glad that you have taken up this cause, as persons as brilliant as my friend should never succumb to suicide.
Can you please submit his name, obituary, and anything else you wish here for confidential registry: https://www.idealmedicalcare.org/contact/ I am so very sorry you have lost your beautiful friend.
Did you compile any information about which psychotropic medications the doctors were using at the time of their death or prior to their death?
A minority.
Regarding my husband Dr. Drummond-Webb:
What broke my heart was the way the medical community in Little Rock, AR tried and succeeded in wiping out all the incredible good he had done. He became defined by his death and not by the incredible life he lived and the thousands of children he saved…… This was reflected 12 years (2016) later by someone in the medical community, I am sure it was a doctor, stopped the sale of our/my house by telling the buyers who had already signed the sale, what happened in the house, and they withdrew immediately. They claimed that they could not raise their 3 children in a house where such a thing happened…… This was AFTER the wife spent 5 hours in the house praying with her bible! Apparently my husband’s ghost was stronger than her god…….!
I should add that the paperwork was done in my maiden name as this is the name I use for practice purposes, which means that whomever told this bariatric Surgeon coming to LR to practice at the Heart Hospital (hospital for adults only) had to have been given Jonathan’s full name – Drummond-Webb to go and search online…… And the address must have been memorized…… After 12 years, this also shows the incredible jealousy Jonathan had to contend with…….
Dr. Lorriane De Blanche
Sending so much love to you. I worked at ACH as an RN in the CVICU and as a CRNA in the main operating room. Your husband contributed so much to the hospital and the children of Arkansas and should be remembered as such.
I read about compassion, lack of privacy, cultural norms, etc. and I did not hear anything about doctors taking control of the medical delivery process and take it back from the hands of the insurance companies and the federal government. How about some compassion, privacy and cultural norms for the privacy of your patient’s and their medical records. You cry about doctor not being able to get confidential mental health treatment. Not one patient has the right to keep their medical records private whether it is mental health or physical health, our records are an open book. Where is your concern about the patient’s right to privacy? Why are you so concerned about doctors? How about some empathy for what you are doing to your patients by taking photos of surgery, exams, etc. and placing them onto HIO servers to be hacked by people making money off the dark web? All medical organizations supported the use of online records and now any doctor, hospital, lab, x-ray, gurney pusher or janitor can view any and all medical records, unless they are doctor’s records, then they are protected. Narcissist much?
After working as a physician since graduating in 1987 I believe that one of the reasons why physicians are unhappy, depressed and increasingly suicidal is the (1) lack of support we give each other, and, in my opinion, even worse, (2) the constant and relentless gossip we have about each other.
The direct, or indirect judgment and gossip not in earshot by the person who is being gossiped about…..
…..that “he/she is a bad doctor/not a good doctor/did you see what he/she did/didn’t do for that patient, haven’t you heard that so-and-so did this-or-that or made such a stupid decision about ‘this-or-that’ – can you believe they did that?
…… and, when there is an adverse event for a patient, no matter how devoted we are, no matter what the relationship we had for a patient, no matter how long term we were that person’s doctor – “medical rounds” or “morbidity and mortality rounds” are more like a systematic means of beating what is left of a doctor’s personality into the ground.
It is rare, that over the decades that I have practiced, that I have heard another doctor praise another doctor – when things go well – nothing for each other – and when things go badly, morbidity and mortality rounds are ruthless grounds for beating the hell out of what is left of the doctor’s personality, ego and, most of all, love for him or herself and/or love for his/her profession.
So that’s my two and a half cents.
Zach
My friend from intern year committed suicide on 4/17/19. There is no news article or mention of her death anywhere including from her anesthesiology residency. She mentioned the stress from in-service training exams and being sexually harassed by a married attending as stressors.
I know who you are referring to. So tragic. I’ll email you.
Pamela can you tell us the ages of the physicians in your “database” (although it sounds cold to call it that) who have completed suicide? The physician in our hospital who completed suicide was well into practice as an attending surgeon. I am looking for better understanding of prevalence among physicians who have completed residency and are in practice. We have had several residents attempt suicide but thank goodness did not complete. Thanks – Mary W (withholding last name for privacy of the colleague mentioned above).
I want to send you an e-mail but don’t want to risk any chance of being identified on the web-site. How do I do that?
Through my contact page here (confidential).
I’m 62 now and retired. I’m an Ivy League trained physician and suffered a lot of reverse discrimination because of that. I
had a head injury in the military as a young man that left me with bipolar illness.
Going through med school and residency was hell for me as I was treated like shit. I was an excellent physician but thought on suicide often. I learned to hate doctors.
Have you heard of a place called Marshfield Clinic in Marshfield WI? They abuse the hell out of physicians on staff and even allow MA’s to refill scripts for dangerous combinations of opiates, including high doses of Chinese fentanyl using the doctors’ signatures without their knowledge or consent. Their physician and nurse turnover is astronomical, and there has even been one recent physician suicide there. The victim was a young female pediatrician … probably an American citizen, since they treat citizens even worse than visa holders.
They need something to live for!
Who cares? I certainly do not. After what these physicians have done to me? Seriously? You know, if I wasn’t stereo-typed by these assholes in white lab coats & scrubs, cut off opioids after 35 years straight of as many as I could swallow literally, then dissed like a bad disease because I’m a dreaded chronic pain patient(pardon the pun), I might have a speck of respect for them…but, as it worked out, I don’t. 1298 is bad…but not bad enough. If they don’t care about me, then why should I care about them? And please do not try and convince me that any of the give a rat’s stinky arse about what I think. Well, they should…
Most doctors enter medicine to help and heal others. Humanitarians. There are easier ways to make money. Believe me.
I see you wont let me post my comment, truth can hurt. Most doctors became a doctor to be called a doctor. They are mostly crooks who think the are better than their patients. Their billing practice should put most of them in jail!
Ill buy the rope for any doctor.
I am a Neonatal nurse Practitioner currently working Locum assignments to survive the evil in medicine. I chose to bring kindness, support, positive energy and encouragement where ever I go. It’s how I choose to make a difference. It’s how I survive. I worked at the Med center for 16 years. I believe in karma and believe in being kind. I stayed longer through all the abuse and bullying at the residents request. They begged me to stay as everyone was leaving. I was always there for them even when the system was not. I treated when with clear unit expectations, kindness support and motherly love. I stayed till the system pushed me out as I would not confirm to being unkind and awful to another human being. I now Work assignments across the US in Levels I-IV. I meet many medical students residents and physicians in all levels of dispair. All trying to survive this life path we are given.
I call that a poor start. Most of these doctors should not be doctors especially hindis as they are assumptive and only understand what they read in a text book to be THE possibility no matter what you tell them actually occurred in your lifetime. They assume all patients to be liars while they themselves feign intelligence. They are rude, inattentive, judgemental and should NEVER be doctors as they are self righteous and assume they know more about your body than you do. If they can’t force you to lie about yourself, they will make it up anyway because their narcissistic personalities tells them that Americans are stupid, liars, alcoholics, and drug abusers. I encourage everyone who has or had a hindi doctor to read their files and remove all the unproven assumptive lies and get a new doctor.
hi,
i will say the issues is larger, these doctors committing suicide most likley do not like working in the framework that is available, corrupt doctors and abusers are not criminally or civiley prosecuted and the nurses etc can be fired for wrongdoing so how would this work environment be in the private world if nobody got fired for wrongdoing??????
I could write an entire essay on this: “After being invited by the AMA to deliver my TEDMED talk, I was disinvited shortly before the event because they were “uncomfortable” with physician suicide.” What a deplorable outrage. Keep going. You will get to them. Hopefully, before the subject gets to themselves.
Doctors are some of the worst people I have ever met. It seems most of these so-called doctors, became a dr. just so they could be called a doctor.
I recently had an experience with an ENT so-called specialist. This man triple booked appointments every time I was there to see him, four times. Waited over a hour to see him for five minutes. It seemed like his most important patient was his next, always in a rush. (being he was behind due to triple booking appointments)
After surgery I told the Dr. that not much has changed in my condition. He told me there was nothing he could do. I then asked about his lack of effort in my diagnosis and he said, “If you don’t like it get the hell out of here, get the hell out of here.”
These doctors pray on sick people and get what they deserve, eventually. So be it if it comes by their own hand!
I will not go into the dishonest, at best, billing practices of these doctors.
Pam,
I am one of those doctors screwed over by a PHP program. I was in residency in 2006. I suffer from chronic pain and I took a corticosteroid from the supply by using a pt’s information. I have Reiter’s and have had seven surgeries for the pain. I was desperate and impulsive. I was fired by my program and reported to a PHP program which stated I was impaired. That destroyed my career. I was forced into the php program or they threatened to report me to the board who would take the license forcibly. I had no options and I signed the paperwork. I lost everything. I was unable to finish my residency, my wife had an affair and we divorced. I wound up being unable to get work anywhere bc of the impairment and not having finished a residency. I had some very rough years after that and I made a bad decision and violated my probationary agreement with the state. However, the agreement was predicated on a lie–I was never impaired nor did I abuse drugs. I was left to rot in chronic pain. Anyway, I recieved a felony for this and I lost my license in Ohio. I am about to punished in Fl and everyday, I think about ending my life. I call myself a coward because I can’t seem to go thru with it. I have children but I don’t know if being around and angry all the time does more harm than good. I am 46 and I have no retirement, I am unable to work in the profession as I am not boarded and have this huge scarlet letter on me.
I don’t know what to do. I fell like switching professions but I have applied for jobs outside of medicine and I cant seem to find anyone willing to hire me. I have many more reasons than anyone else to commit suicide and I get closer and closer every day. I have a colleague who went thru something like this in his life as well. We found that these php’s will report everyone as impaired. And while maybe it doesn’t cause chaos in some people’s life because they are lucky, the one’s who do get hurt are maimed and killed for it. I wish the state would just take care of me. I wouldn’t have to commit suicide if they just put me on death row. I would welcome it and I wouldn’t fight their decision. I would welcome it.
Oh this is terrible. If I had your real email I’d get in touch personally. I will respond here with some ideas. One option would be to join our physician trauma support group.
As always, I’m here to talk.
I appreciate the concern. I really do, but I don’t know how to go about fighting the states who have immunity against their actions and take prn’s word as gospel and wont take non-board approved evaluations. Ohio, MO, FL- they don’t care about me and they dont want to listen to me. They probably hope I commit suicide. They have to be saying what insane idiot would spend this much time to fight us–doesn’t he know we are going to destroy his reputatoin, his career, and his sanity. They hide behind the veil of “patient safety” and rationalize the extreme overkill as trying to keep the public safe from bad doctors, while in actuality they destroy doctors with impugnity. My voice was lost the minute I was sent to the impairment program. I admit I have made my share of mistakes, but the states have all ignored my actual auto-immune disorder which has been confirmed by at least 10-15 MRI’s,Extensive labwork and 7 surgeries. My medical history was ignored and didn’t even get a cursory glance. Instead, I was forever labeled a corticosteroid addict despite telling the counselors my nedically necessary mediciatins and need for the meds prescribed (self prescribed elavil, tramadol(before scheduled drug). They condemned me to the gallows as a drug abuser a, liar, and unethical.They also gloss over 9 years of monitoring that was without incident except to travel to lebanon. I didn’t ask for permssion because I hated the disparate treatement I received while being labeled an addict and not w the c heronic disease condition. I know a resident who finished his 3rd year and now enjoyed his best life. He has his health, wealth, and happiness.
I thought I’m going to travel and see my faimily as this will likely be outside of the country,I’ll leave a sample which could be sent in. I just want someone on any one of these boards to listen to me for 10 minutes so I can tell them the hell that I have endured and how I can be successfully rehabilitated and trained. But they don’t want to be seen as soft on drugs so let the punishment and pain continue, I’m GOD’s special whipping boy. Maybe just maybe (If GOD stops punishing me for all of one day)they will see the truth–that these impairment programs make unsubstantiated allegations purely for a profit motive and cause cruel and unusual punishment on doctors and ruin the doctor’s lives as well as their family. The trauma reverberated thru my family. My parents and my siblings all know the pain I have suffered. There have been so many nites of crying and telling them that I wanted to end the pain. They would always say have hope but they also stopped calling bc all my stories would end in seething hatred of the medical board in OHIO. The
board would say Stay strong and I’d tell them I had issues getting work. The non physicain member of the board, Mr. Albert would tell me to go back to residency. Well, I tried that when I was booted from my anesthesia residency. I called every D.O. program in the countrty and no one would help. I called the AAOA, they didn’t want to help. No one wanted me to succeed. So I have no work options, I’m paying 150/month for monitoring my uirne now going on the better part of two years(2006-2008) and I get the final divorce papers from my ex-wife. I am beyond pissed and I was depressed and nothing is working out. My reis gone. And when your relationship dissolves, people generally throw themselves into work. Well that’s a no. And I can’t go to the gym because my foot was still hurting. It’s an absolute nitemare. I had to move in to section 8 housing for f @ 1 year.I am unable to get medicare as they stated my felony was detrimental to the medicare beneficiarys. Multiple medical coding jobs have turned me down. The only way I have been able to work is I started my own urgent care but it’s limited bc i can’t see Medicare/MA. I honestly think the only way I could
Please see the very comprehensive piece I did on Physician-Friendly States for Mental Health: A Review of Medical Boards. May help you. Some state are far better than others.
Thank you,
I’ll take a look. I have a board hearing on the 15th of Nov for another board who wants to take action against my license. This is all overkill. I have seething hatred for these regulatory agencies who base their decisions on a punitive model. What’s infuriating is the united states has one of the worst criminal justice systems and the punitive model has been found to be unsustainable. The consensus is that by providing hope and skills for recover, it helps build people to be productive members of society so they do not repeat crimes. IF you take that away, then people become hopeless and become impulsive and self-destructive. Doctor’s included. My wifes family is the lead on the class action lawsuit against the michigan physician health program and I hope they take down these awful, horrible cancers upon the profession. Everyone of these agencies should be evaluated for their predatory behaviors (30K or they tell the state and sign an agreement or lose your license), their complete over-reach and wildly abnormal addiction rate amongst professionals. (I heard the facilities where doctors were sent found 100% of professionals were impaired, far higher than statistical norms). And Finally, total lack of regard for medical records which might exonerate someone. If this was a police investigation, it would have been inadmissible because of the gross oversight but because these facilities had been board approved, they could make these wild accusations and now their word meant more than mine. As a resident without income, my funds were depleted and I had no choice but to sign to return to any semblance of work. What is a crazy twist is Ohio had already handed my license back to me in aug 2006, I was working as an ER physician in a rural ER in MO but I was able to support my wife and myself. However, MO state board required a MO board approved program thus I had to see Rush who then said I was unethical and was a risk to pt’s. So despite having been seen by Ohio physic +ians who were acceptable to the state of Ohio and found no ethical issues, Rush destroyed my MO license even though I had been working for almost 6 months. When MO PhP, they said never use Rush as Rush was a bunch of dicks, I didn’t know. Does anyone hear see the lunacy? I’m trying to keep a job in order to use my medical skills and maybe get my life back on track, but no, Rush decided more pain was necessary, more punishment because that was the key to help me build hope for the future. So If anyone is reading this, just know, the boards are the product of the devil and they should be shut down or severely restricted. They are based on a flawed model and use quasi research and anectodal evidence (five years of monitoring) to justify the program.
I’m giving a keynote in November in NY. The woman speaking before me represents the NY Medical Board who will be revealing 49 ways to lose your medical license. Here’s what was posted in Twitter: “Did you know that it is professional misconduct in NY if a physician is not wearing an ID in a hospital, clinic, or group practice? Find out the other 48 ways to lose your medical license at NYCOMEC’s Grand Rounds on November 20th.” What fun! I never knew there was a list of 49 ways to lose a medical license. What about 49 ways to support your suicidal colleagues? That might be a great talk!
I recently retired at age 50. I am fortunate to have the resources to do that.
I have two lovely children. I have little else.
My husband left me, most friends too. I don’t have much of a personality– that left too. I am sure that I am exceptionally uninteresting outside the office.
I know little outside of medicine.
I am embarrassed of my lack of time and knowledge. I can’t discuss current events because I never had time to read long articles or understand them. I can’t discuss movies or films because I didn’t have time to see them.
I have been a single parent for 12 years and physician for 23 years.
My life was 1)work 2)time with kids (usually thinking about work the whole time)
nothing else.
I have not gone to lunch with a friend. I have not gone to dinner with friends. I have not read the paper. I have not read a book. I have not been to exercise class or a mommy group or a book club. I have not read a non-medical book in twenty years.
I feel like I was just released from prison and am now twenty years behind.
I feel almost cripplingly inadequate and ignorant about any field outside medicine. I am at a loss to explain this to non-medical people.
I have never had a physician friend in any way. We cannot befriend patients (and we don’t want to, they all just want something), we cannot befriend other doctors, and we have no time for anything else. I am a excellent physician. I also am NOTHING else.
I don’t even really know if I am liberal or conservative. Even major events over the past 23 years are hazy. I have SO MUCH work to do to catch up, to feel like “a person”.To have opinions on things not related to medicine. I am so very dull.
I am embarrassed to interact in the “real world”. I KNOW how to care for people. I don’t know how to discuss politics or sports or anything else. I am tired of hiding all of this in shame. Tired of trying to “be interesting” when in fact I am not.
I would really love to speak with you. Have actually felt the same way myself at times. Very common these feelings. I sent you a personal email. Looking forward to speaking to you.
Hello,
I’m currently working on suicide rates among physicians for my PhD in France. Do you have the datas or the references from the study about the suicide rates in 1858 ? I can’t find it…
Thnak you and thanks for your work
I think the reason why doctors commit suicide is because you either cannnot say or this is beyond your comprehension that doctors may be being killed and looks like a suicide. Why has the medical profession been so impacted by ed myers, the prime mover, I suspect, to insert abducted people into the medical practice who have to do tricks for him to the patients, a very sick and dangerous man with a JHH degree in English, graduate level. Simply put, I suspect this man has obversions to kill, very conveniently, for the depopulationists. Happiest people are often holiest people and they are one group targeted by these devils. You need to start polygraphing more doctors upon admittance to schools and hospital staffs if there is not a true credentialed person, especially. Perhaps some doctors do find out some secret agenda of the most honorable profession, and commit suicide because of that. Oh and by the way, many tens of thousands of professional staff have been shipped or flown out to foreign countries, non European countries, mostly todo science as a white slave.
Malpractice suits kill doctors?
Don’t make me laugh.
MALPRACTICE kills PATIENTS.
We who doctors have murdered and maimed do not deserve to be guilted over suing.
If this is your takeaway, please retire both from medicine and
journalism.
Pamela,
Thank you for the your courage and compassion, and especially passion to champion his problem. As a suicide survivor from the early 1990s, I’ve managed to clean up the severe collateral damage and returned to work as a physician. I am soon to retire and write a book about it (I would never attempt that with an active license). Your website and references are not only inspiring but resources I will share in my book and with other doctors. If there is one thing I could offer as most important in reducing physician suicidality, it is to strengthen personal boundaries and say “no,” which is opposite of what we are expected to do. I believe that the inability to say “no” to the constant demands is what most often kills us. It took me years to figure out how to do that. I’ll be following along. Thank you.
Good morning.
My name is Dr. Kelly Logan a physical medicine and rehabilitation physician in Kansas City, Mo. I am an advocate for physician health, mental health and teaching meditation and self care to healthcare professionals.
I would be very interested in connecting with you to further this movement.
Started and led a hospitalist program at a rural critical access hospital created to fix the primary care physician burnout problem. Despite great success of the program, state legislators cut funding to the now only 5 star Medicare rated hospital in the state. When I tried to show the new CEO and Board all the benefits, the program now 10 years old, was cut from the consultant recommended 3.6 FTE to 2 FTE leaving us covering 25 beds including a 4 bed ICU. Med staff fought against eachother to avoid further cuts of their staff. No one would stand up to the narcissistic CEO (as described by others not myself). I found myself demoted in attempts to explain to everyone that 24/7 shifts were not safe. I documented bad patient outcomes and sent them to the new quality nurse (the prior one left angry with the unsafe culture created) A new director was hired in my place and she was adamant followed the marching orders of the new CEO who publicly disgraced any resisting physicians. Instead of cuts occurring across the whole system, higher paid physicians were targeted to address the initial $3 million Funding cut and there were no supporters from nursing or elsewhere to support distress physician programs since no one wanted to become the next victim of the CEO who was given unchecked power of the bullying CEO.
As I tried to comply with the new program in efforts to provide excellent care to the community And native population I loved, I found myself working shifts with average of 3 to no sleep over days, received for the first time in my career repeated degrading feedback from the director who assumed my role, for the first time began getting behind in completion of my records, had several times falling asleep at the wheel, became depressed with thoughts of self harm and worst of all, witnessed repeated poor outcomes that included major mistakes made by the new director which when I tried to expose all the problems, she commented that “there is a time for people to die” and “people get old and need to retire” (referring to me at age 65). Other physicians labeled her “Dr Death” yet no one was willing to expose what was happening. When I fell asleep driving home the 3rd time and reported the problem to her and the now 3rd CEO, I was told I would no longer be on the schedule but instead be offered to do Long term care. The director told everyone that I was unsafe and incompetent which clearly is not the case. I gave outstanding care. Everyone is afraid to speak out against an entrenched administration. I tried to give excellent care under conditions that are very unsafe. The directors response to my concerns, “you know, we have to take care of ourselves first”. And that she does as she takes in $300K to support a program that goes on hurting many patients she never reports despite being on the peer review committee. What a humiliating ending to the marked effort I gave to the community and the final moments of my career. Prior to the funding cuts, I was praised for the program that saved the primary care physicians careers and well being while propelling the critical access hospital to be the only 5 star Medicare rated hospital in the state. Within a year of the financial distress and departure of the team I hired, we were rated 3 of 5. Repeated bad administrative decisions resulted in 2 new EHR installs In 5 years, both of poor and less expensive systems. Bad outcomes are ignored as the hospitalist director oversees the programs quality and fails to report her own horrible mistakes and people like me are tossed aside as inadequate and incompetent. Suicidal thoughts have occurred many times since my demotion in 2016 which was the year of our 5 star rating and angered departure of our quality nurse who was abhorred with the changes being made.
Hi Pam – you did a great job talking at our AO surgeons conference in Phoenix last weekend. It brings to light a problem that you have “pulled the covers off of” and are willing to stand up and educate others about. Congratulations and keep working at it – you are making a difference.
Rick Buckley
Oh thank you so much Rick. I’ve got the whole talk transcribed with slides, audio & video here: https://www.idealmedicalcare.org/creating-a-culture-of-wellness-keynote/
Dr. Wible, I am not a doc and I am not even in medical industry. However, I feel like this is a self-inflicted wound. Existing physicians design a system to intentionally limit the production number of medical students. Existing interest groups are intentionally design the curriculum to make this route harder. In Asian/European countries, their high school graduates could directly go to law schools/medical schools and become a lawyer within 4 years or become a doc within 5 years. You do not need to get a bachelor degree before going to med school. The medical board exam is easier in other countries. Anyway, if government is not willing to break up those interest groups, American society will continue to suffer expensive but mediocre quality health care and this kind of suicidal cases will continue to happen.
Thanks John. Criminals hide in complexity and organized crime has taken over aspects of medicine in US. Really tragic. Agree that oftentimes our leaders in medicine have sold us out. The profiteering infrastructure that has grown up around the healing profession must be taken down.
I got bullied for 13 years in a very hostile Male dominated department. As soon as I hired an executive coach and started speaking up, i got fired. No reason given. Just told to leave. All i think about is how to not bed in so much pain and that my kids would at least have my insurance money since i don’t work.
Please forward me t he ones you know about on covid-19 you sent an email but i accidentally deleted it
Most are listed here: Honoring those we lost to suicide amid COVID-19
All of this said in Dr. Wible’s video is so true and abuse in the medical field and abuse in every field needs to stop.There is absolutely no excuse for abuse in the workplace under any circumstances. Abuse leads to mental health issues and even can cause suicide. Medicine is a hard enough profession without having to be abused on a daily basis. There is absolutely no excuse for any abuse in any workplace. As a victim of workplace abuse as a doctor, I will always stand up against abuse. The doctors that are abusing others need to focus on saving patients lives and their patients instead of horrific abuse that is leading to suicide in some cases. Thank God for Dr. Wible shining a light on these issues.
The genesis of the abuse in medicine is intergenerational wounding due to vicarious trauma and punishment for seeking mental health care.
The issue of suicide method is important to document. I recently published an article about trauma centers and self inflicted gunshots. The ease of successfully committing suicide with a gun contrasts with other methods. Gun violence is a very popular topic–and it’s commonly stated that 2/3 of gun deaths are from suicide. There is even group of surgeons who are gun owners that are the ones writing the proposals for gun policy by the ACS…it’s a little odd.
While married to my first husband who at the time had recently begun the 1st year of emergency medicine residency he said one morning ” I wish I could cross _____ street and get hit by a truck.” He refused to seek help for all the reasons already mentioned here but in retrospect had been attempting to self medicate bipolar or depression with alcohol for years before that. He remarried a woman 15 years younger and when a few years ago I happened upon his 2015 obit saying simply he “passed away ” at age 59 I thought I wouldn’t be surprised if the COD was suicide. Mental health issues were viewed as weaknesses that could not be admitted, let alone discussed. In his 4th year of medicine school he did tell me he chose EM as a specialty so he wouldn’t be bothered with regular patients problems all the time like he would if he was practicing peds,family medicine etc.
So sad Roberta. Have you seen the film Do No Harm that exposes the doctor suicide crisis? On Amazon here: https://donoharmfilm.com
This made me burst into tears. “Medical school killed half my family” rings so familiar. Medical school ruined my life. It hurts a lot. And although I was forced, against my will, to stay alive when I was laying out the pills for my suicide two years ago, SOMEBODY died then. The enthusiastic, bold person I was is long dead. Thanks, medicine.
I feel your pain. Likely the majority of docs do as well. Free ebook explains the soul sacrifice: Physician cycle of betrayal and abuse is extreme.
Thank you for drawing much needed public attention to this crisis.
There is a ripple effect from the trauma of physician suicides.
Their family will never recover.
My son is a surgery resident and has been intermittently suicidal for years. I hope and pray that he survives. He will wind up with PTSD, so will I and, if the relationship lasts, his wonderfully supportive partner.
Doctors also know that much of the medication they’re prescribing causes far more harm than good. Try going against Big Pharma…
Suicide only becomes a viable option when the pain of life becomes unbearable. Think about it for a moment. Death is the end of life. Who could possibly want to die let alone take thier own life? Well a lot of people based on the statistics. People think Suicide is like fliping a light switch. If I turn it off the light will end. So it goes if I kill myself the pain will end. Emotional pain is as bad or worse than physical pain. Physical pain can be addressed in most cases by the right treatment. So too can suicide but it is very difficult to tell loved ones we are emotionally sick because it often goes unseen. If I lose a leg it is obvious to all. Depression goes unseen often for many years. We have to end the stigma of seeking mental health assitance so fewer people see suicide as a viable option. Remember if you kill yourself you may no longer feel any pain but those that you love who you leave behind will feel that pain forever.
I wanted to share a thought as to why a doctor might pick hospital setting for suicide: in hopes the medical person who finds them is less traumatized than a “civilian” would be, to preserve the family home, and to lessen the chaos/burden around transport and clean up of their body. I’ve followed your work for several years. It is so important. Blessing to cover you and many thanks
Thank you for your touching TED Talk. Awesome! I have a biking buddy Doctor I am going to share it with.
This is concerning but so too are the numbers of those with chronic pain who have suicided because they are no longer able to get the pain meds that had been helping them due to fear of the CDC and them misinterpretation of the CDC opioid “guidance.
As well as the trouble many find in finding a doctor who is willing to manage their pain.
Thank you for doing all that important work. The director of the ED where I worked happily for many years shot himself. The ED went downhill after that because he was wonderful. I had to leave and now commute hundreds of miles to work. It’s a HUGE problem. His name was Oscar molar. He was the director of the ED in Taos New Mexico. We were all devastated. Also, when I was in medical school at ucsf there was a resident who jumped out of a window. He did not survive. One thing I think is important to mention is the fact that the nurses can really make one’s life miserable. Sometimes they are mean, spread rumors and make inappropriate comments. They can be vicious. And, the amount of effort it takes to keep up with cmes and boards is ridiculous. Our system is broken. Hospitals are run by business people who know nothing about medicine. They make decisions that are wrong. I have many stories about things that have happened that are totally inappropriate. I understand why people take their lives. Sometimes it feels like too much. That you will never be good enough. See patients fast and don’t relate. But that’s the best part. Perfection is expected always. I wish I went into veterinary medicine instead. I think I’d be happier.
I learned today of a doctor who committed suicide after not being able to get benzodiazepines that had been prescribed for years and allowed her to be a great doctor. In a final act of giving she ensured the truth about her passing was known. Often swept under the rug this type of tragedy happens more often than we care to admit. End the War on Drugs & its cousin The War on Pain patients. Sunshine is the best disinfectant. Thank you for allowing others to see the unintended consequences of bad policies that we can change. Allowing doctors to use their education, training and experience with much less supervision by DEA Cops as Docs is an important first step.
Who was the doctor? I know several (at least 4 off the top of my head) who died from benzo withdrawal syndrome.